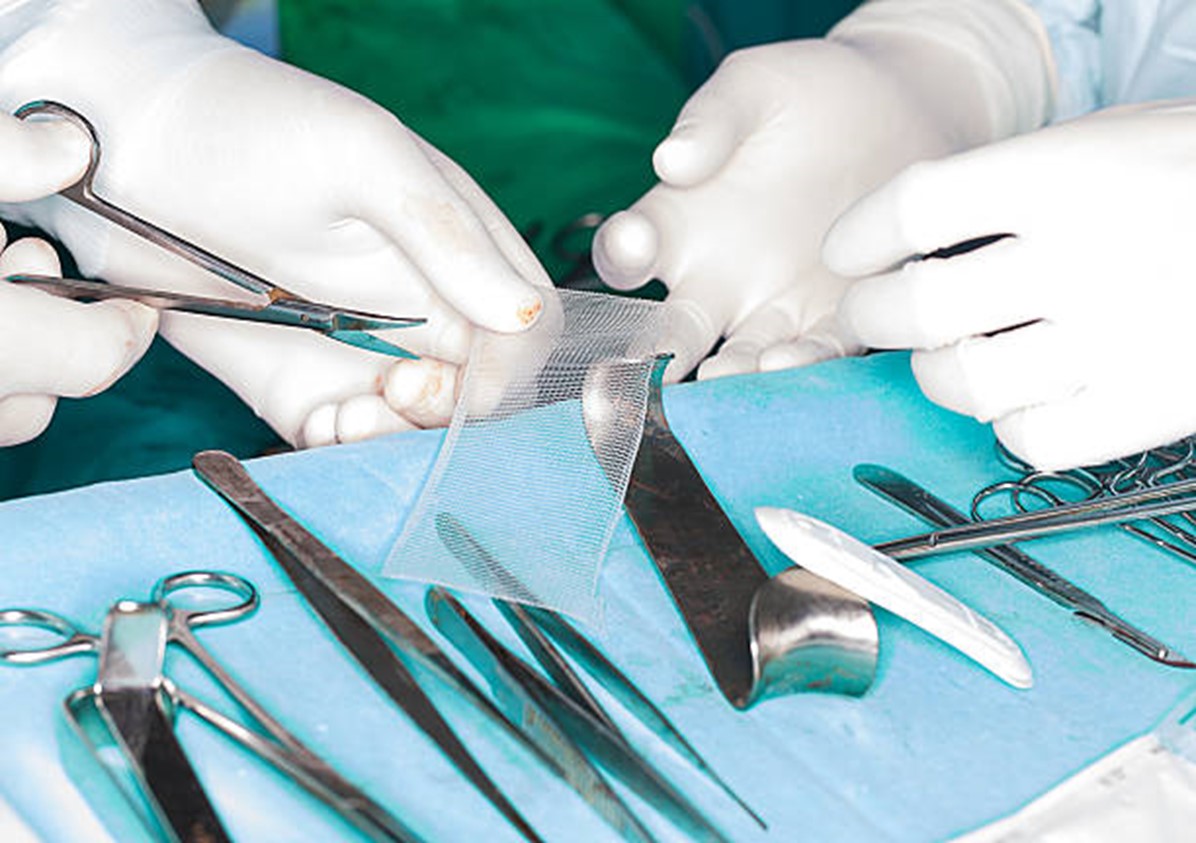
Surgical Mesh Used for Hernia Repair
The FDA is providing information to help people make informed decisions about surgical mesh used for hernia repair. The information includes treatment options, commonly observed complications, and questions to discuss with your health care provider. We have also included a review of certain adverse event reports and instructions for reporting problems to the FDA.
On this page:
- What is a Hernia?
- Types of Hernias
- Causes of Hernias
- Treatment Options for Hernias
- Surgical Mesh
- Additional Resources
What is a Hernia?
A hernia occurs when an organ, intestine or fatty tissue squeezes through a hole or a weak spot in the surrounding muscle or connective tissue. Hernias often occur at the abdominal wall. Sometimes a hernia can be visible as an external bulge particularly when straining or bearing down.
Types of Hernias
The most common types of hernias are:
- Inguinal: occurs in the inner groin
- Femoral: occurs in the upper thigh/outer groin
- Incisional: occurs through an incision or scar in the abdomen
- Ventral: occurs in the general abdominal/ventral wall
- Umbilical: occurs at the belly button
- Hiatal: occurs inside the abdomen, along the upper stomach/diaphragm
Causes of Hernias
Most hernias are caused by a combination of pressure and an opening or weakness of muscle or connective tissue. The pressure pushes an organ or tissue through the opening or weak spot. Sometimes the muscle weakness is present at birth but more often it occurs later in life. Anything that causes an increase in abdominal pressure can cause a hernia, including obesity, lifting heavy objects, diarrhea or constipation, or persistent coughing or sneezing. Poor nutrition, smoking, and overexertion can weaken muscles and contribute to the likelihood of a hernia.
Treatment Options for Hernias
Hernia repairs are common procedures. As many as one million hernia repairs take place each year in the U.S.1 Treatment options for hernias include:
- Non-Surgical Options
- Only 3% to 5% of hernias will require emergency treatment for bowel obstruction and strangulation of trapped organs. Scheduled (that is, non-emergency) surgical treatment will eventually be required in 30% to 65% of hernias.2 If your hernia is not symptomatic, or if you have significant risks for surgery, your surgeon will monitor the hernia and make sure that it is not getting larger or causing problems. The use of abdominal binders and trusses may help minimize your symptoms by keeping the hernia flat.
- Surgical Options
- Laparoscopic repair - The surgeon makes several small incisions in the abdomen that allow surgical tools into the openings to repair the hernia. Laparoscopic surgery can be performed with or without surgical mesh.
- Robotic repair - Like laparoscopic surgery, robotic surgery requires small incisions to repair your hernia. Robotic assisted surgical devices may offer ergonomic benefits for the operating surgeon and technological advances to include motion-scaling, tremor reduction and improved optics including surgeon control of the camera.
- Open Repair - The surgeon makes an incision near the hernia and the weak muscle area is repaired. Open repair can be done with or without surgical mesh. Open repair that uses sutures (stitches) without mesh is referred to as primary closure. Primary closure is commonly used to repair inguinal hernias in infants, small hernias, strangulated or infected hernias.
Surgical Mesh
Surgical mesh is a medical device that is used to provide additional support to weakened or damaged tissue. The majority of surgical mesh devices currently available for use are constructed from synthetic materials or animal tissue.
Surgical mesh made of synthetic materials can be found in knitted mesh or non-knitted sheet forms. The synthetic materials used can be absorbable, non-absorbable or a combination of absorbable and non-absorbable materials.
Animal-derived meshes are made of animal tissue, such as intestine or skin, that has been processed and disinfected to be suitable for use as an implanted device. These animal-derived meshes are absorbable. The majority of tissue used to produce these animal mesh implants are from a pig (porcine) or cow (bovine) source.
Non-absorbable mesh will remain in the body indefinitely but may undergo some degradation over time. It is used to provide permanent reinforcement to the repaired hernia. Absorbable mesh will be absorbed and lose strength over time. It is not intended to provide long-term reinforcement to the repair site. As the material is absorbed, new tissue growth is intended to provide strength to the site of the repair.
Benefits of Surgical Mesh in Hernia Repair Surgery
Hernias have a high likelihood of developing again, and surgeons often use surgical mesh to strengthen the hernia repair and reduce the rate of it happening again. It is generally accepted that most hernia repair surgeries in the U.S. use mesh.3
Information found in medical literature has consistently demonstrated a reduced likelihood of a hernia developing again with the use of mesh. Still, there are situations where the use of surgical mesh for hernia repair may not be recommended. Patients should talk to their surgeons about their specific circumstances and their best options and alternatives for their hernia repair.
The use of surgical mesh may also improve patient outcomes through decreased operative time and minimized recovery time. However, recovery time depends on the type of hernia, the surgical approach (for example, open or laparoscopic surgery), and the patient’s condition both before and after surgery.
Risks of Surgical Mesh in Hernia Repair Surgery
Based on the FDA’s analysis of medical device adverse event reports and of peer-reviewed, scientific literature, the most common adverse events for all surgical repair of hernias—with or without mesh—are pain, infection, hernia recurrence, scar-like tissue that sticks tissues together (adhesion), blockage of the large or small intestine (obstruction), bleeding, abnormal connection between organs, vessels, or intestines (fistula), fluid build-up at the surgical site (seroma), and a hole in neighboring tissues or organs (perforation). For hernia repair with mesh, additional adverse events include migration or shrinkage (contraction) of the mesh itself, which may more likely be associated with the previously mentioned complications of hernia repair.4
Additional Resources
1K. Malhotra and A. Bawa. Prioritizing and Promoting Hernia Awareness Month: A Call for Action. World J Surgery 2022. doi: 10.1007/s00268-022-06553-6.
2D. Kokotovic, H. Sjølander, et al. Watchful waiting as a treatment strategy for patients with a ventral hernia appears to be safe. Hernia 2016; 20(2):281–7. doi: 10.1007/s10029-016-1464-z.
3L. Funk, K. Perry, et al. Current national practice patterns for inpatient management of ventral abdominal wall hernia in the United States. Surg Endosc. 2013; 27(11):4104-12. doi: 10.1007/s00464-013-3075-4.
4D. Kokotovic, T. Bisgaard and F. Helgstrand. Long-term Recurrence and Complications Associated With Elective Incisional Hernia Repair. JAMA 2016; 316 (15):1575-82. doi: 10.1001/jama.2016.15217.