Locally-Acting Orally-Inhaled and Nasal Drug Products
Introduction
Demonstration of therapeutic equivalence for locally-acting orally-inhaled and nasal drug products (OINDPs) presents a unique challenge since the traditional PK approach used for systemically acting drugs is not directly applicable to BE OINDPs, which deliver drug(s) to the site(s) of action in the lung and nose, respectively. Additionally, IVIVC and predictive in vitro methodologies to determine regional deposition and local availability of OINDPs is lacking. Furthermore, systematic understanding is low regarding the effect of active and inactive ingredients and device design on performance of OINDPs.
Research
With the intent to develop BE recommendations for inhaled generic drug products, OGD funded several research projects to develop clinically relevant in vitro methods to enable predictive regional deposition and local bioavailability of OINDPs, assist in assessment of BE, and serve as a pharmaceutical development tool for OINDPs. These projects include research aimed at developing: (1) predictive dissolution methods, (2) predictive lung deposition models, and (3) clinically relevant in vitro performance tests incorporating mouth-throat models for inhalation products. Additional research will study the effect of device design and formulation factors on the performance of dry powder inhalers and metered dose inhalers. Further, OGD has funded an investigational study to explore the feasibility of using exhaled nitric oxide in asthma patients. With the aim of exploring more efficient methodologies to establish the BE of OINDPs, two research studies will assess if PK studies are able to provide information about drug fate at local sites of action in the lung and nose for dry powder inhalers (DPI) and nasal suspensions, respectively.
Figure 10. Particle impaction velocity in: (A) Accuhaler® and (A') Multihaler® DPI device at 60 L/min
Particle simulation is 30 μm in both devices. Reproduced from Shur J, Saluja B, Lee SL, Tibbatts J, Price R. Effect of device design and formulation on the in vitro comparability for multi-unit dose dry powder inhalers. AAPS J. In press (2015)
Figure 11. "Realistic" mouth throat models and USP inlet
From left: Oropharyngeal Consortium (OPC) Large; OPC Medium; OPC Small; Virginia Commonwealth University (VCU) Large; VCU Medium; VCU Small; Alberta Idealized Throat. Reproduced from Byron PR et al, Proceedings of Respiratory Drug Delivery Europe 2013, Volume 1, 2013: 85-92 with permission from RDD Online and Virginia Commonwealth University
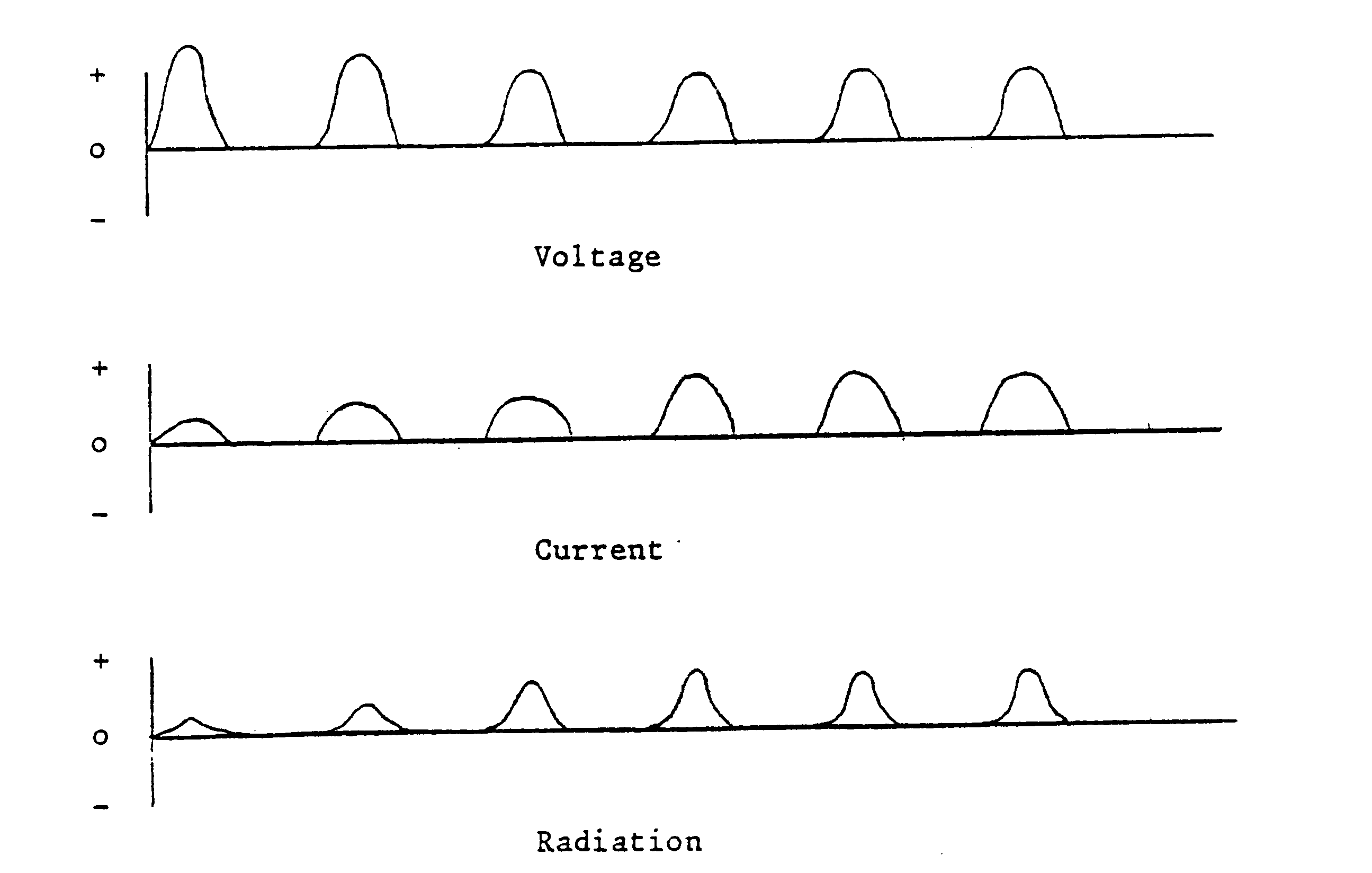
Figure 12. Probability of passing methacholine-induced bronchoprovocation bioequivalence study
(A) Probability of passing methacholine-induced bronchoprovocation BE study as a function of the F ratio, number of subjects (N), and BE limit; BE limit of 80.00-125.00%;
(B) BE limit of 67.00-150.00%. Published with permission from Respiratory Drug Delivery 2014, Virginia Commonwealth University and RDD Online; Saluja B, Delvadia RR, Kim SH, Lee, SL. Evaluation of bioequivalence criteria for methacholine-induced bronchoprovocation: bioequivalence study of albuterol sulfate metered dose inhalers, Respiratory Drug Delivery, Volume 2, 2014:413–416 (2014)
ORS staff facilitating research in this area
- Bhawana Saluja, Mohammad Absar, Denise Conti, Renish Delvadia
Projects and Collaborators
- Development of Clinically Relevant in Vitro Performance Test for Generic OIDPs
- Site PI: Michael Hindle (Virginia Commonwealth University)
- Grant #: 1U01FD005231-01
- Comprehensive Evaluation of Formulation Effects on Metered Dose Inhaler Performance
- Site PI: Guenther Hochhaus (University of Florida)
- Grant #: 1U01FD004943-01
- An optimized dissolution test system for orally inhaled drugs: development and Validation
- Site PI: Guenther Hochhaus (University of Florida)
- Grant #: 1U01FD004950-01
- In vitro fluid capacity-limited dissolution testing and its kinetic relation to in vivo clinical pharmacokinetics for orally inhaled drug products
- Site PI: Masahiro Sakagami (Virginia Commonwealth University)
- Grant #: 1U01FD004941-01
- Development of in vivo predictive dissolution technique to understand the clinical based
- Site PI: Robert Price (University of Bath)
- Grant #: 1U01FD004953-01
- Study to investigate the sensitivity of pharmacokinetics in detecting differences in physicochemical properties of the active in suspension nasal products for local action
- Study PI: Guenther Hochhaus (University of Florida)
- Contract #: HHSF223201310220C
- Pharmacokinetic research study on the effects of different protective packaging on the stability of fluticasone propionate capsules for inhalation
- Study PI: Guenther Hochhaus (University of Florida)
- Contract #: HHSF223201300479A
- Evaluation of formulation and device changes on in vitro performance of dry powder inhaler (DPI)
- Study PI: Robert Price (University of Bath)
- Contract #: HHSF223200910017C
- Quality by design of orally inhaled drug products: chemistry, manufacturing and controls
- Study PI: Robert Price (University of Bath)
- Grant #: 1U01FD004321-01
Publications and Presentations
- Azimi M et al. Towards clinically relevant in vitro testing of locally acting nasal spray suspension products. Proceedings of Respiratory Drug Delivery (RDD), Davis Healthcare International, River Grove IL (2015)
- Sakagami M. Fluticasone pharmacokinetics: meta-analysis and models. Proceedings of RDD, Davis Healthcare International, River Grove IL (2014)
- Saluja B, Delvadia RR, Kim SH, Lee, S. Evaluation of bioequivalence criteria for methacholine-induced bronchoprovocation bioequivalence study of albuterol sulfate metered dose inhalers. Proceedings of RDD, Davis Healthcare International, River Grove IL (2014)
- Saluja B, Li B, Lee S. Bioequivalence of orally inhaled and nasal drug products. FDA Bioequivalence Standards, New York NY: Springer (2014)
- Depasquale R, Lee SL, Saluja B, Shur J, Price R. The influence of secondary processing on the structural relaxation dynamics of fluticasone propionate. AAPS PharmSciTech. Epub ahead of print (2014)
- Shur J, Saluja B, Lee SL, Tibbatts J, Price R. Effect of device design and formulation on the in vitro comparability for multi-unit dose dry powder inhalers. AAPS J. In press (2015)
- Shur J, Lee SL, Adams W, Lionberger R, Tibbatts J, Price R. Effect of device design and the in vitro performance comparability for capsule-based dry powder inhalers. AAPS J. 14(4):667-676 (2014)
- Tian G, Hindle M, Lee S, Longest PW. Validating CFD predictions of pharmaceutical aerosol deposition with in vivo data. Pharm Res. DOI 10.1007/s11095-015-1695-1 (2015)
- Dalasm N K H and Longest PW. Deposition of particles in the alveolar airways: inhalation and breath-hold with pharmaceutical aerosols. J Aerosol Sci 79:15-30 (2015)
- Walenga R L, Tian G, Longest PW. Development of characteristic upper tracheobronchial airway models for testing pharmaceutical aerosol delivery. American Society of Mechanical Engineers (ASME) Journal of Biomechanical Engineering [2.1] 135(9), 091010 (2013)
- Holbrook LT and Longest PW. Validating CFD predictions of highly localized aerosol deposition in airway models: in vitro data and effects of surface properties. J Aerosol Sci [2.8]. 59:6-21 (2013)
- Longest PW, Tian G, Delvadia R, Hindle M. Development of a stochastic individual path (SIP) model for predicting the deposition of pharmaceutical aerosols: effects of turbulence, polydisperse aerosol size, and evaluation of multiple lung lobes. Aerosol Sci Technol [3.2]. 46(12):1271-1285 (2012)
- Longest PW and Holbrook LT. In silico models of aerosol delivery to the respiratory tract – development and applications. Adv Drug Deliv Rev [12.1]. 64:296-311 (2012)
- Longest PW, Tian G, Walenga RL, Hindle M. Comparing MDI and DPI aerosol deposition using in vitro experiments and an new stochastic individual path (SIP) model of the conducting airways. Pharm Res [4.5]. 29 1670-1688 (2012)
- Tian G, Longest PW, Su G, Walenga RL, Hindle M. Development of a stochastic individual path (SIP) model for predicting the tracheobronchial deposition of pharmaceutical aerosols: effects of transient inhalation and sampling the airways. J Aerosol Sci [3.0]. 42:781-799 (2011)
- Schroeter JD, Holt JT, Asgharian B, Bovet JM, Hickey, AJ. Characterization of Particle Size Distributions and Respiratory Tract Deposition of Albuterol Sulfate Metered Dose Inhalers. Proceedings of RDD, Davis Healthcare International, River Grove IL (2014)
- Mitran S, Hickey AJ, Holt JT. Multilinear calibration of lattice boltzmann pMDI spray simulation. Proceedings of RDD, Davis Healthcare International, River Grove IL (2014)
- Holt JT, Hickey AJ, Sandell D. From Q2 to QbD: the influence of formulation changes on MDI performance. Proceedings of RDD Asia, Davis Healthcare International, River Grove IL (2014)
Outcomes
- Product-specific recommendations for fluticasone propionate/salmeterol xinafoate powder for inhalation
- Product-specific recommendations for albuterol sulfate metered inhalation aerosol
- Product-specific recommendations for levalbuterol tartarate metered inhalation aerosol
- Product-specific recommendations for ipratropium bromide metered inhalation aerosol

