2023 FDA Science Forum
Using microfluidics to assess thrombus formation caused by abuse-deterrent opioid tablet formulations administered via a non-intended intravenous route
- Authors:
- Center:
-
Contributing OfficeCenter for Devices and Radiological Health
Abstract
Background:
The abuse of prescribed opioids is a major public health issue. Abuse-deterrent formulations (ADFs), such as tablets containing high molecular weight (HMW) polyethylene oxide (PEO), were developed for opioids to alleviate this issue. However, case reports reveal recurring safety issues when abusers intravenously inject opioids with PEO excipient. Complications include microangiopathic hemolytic anemia, thrombocytopenia, and renal failure with thrombosis observed in the kidneys, though the mechanism by which PEO causes aberrant thrombosis is unknown. The development of microfluidic models to simulate blood flow in capillaries can help in the understanding and prevention of thrombotic events thought to be associated with adulterated opioid intravenous injection.
Purpose:
This cross-cutting, collaborative effort is intended to elucidate the relationship between tablet excipients, manufacturing and manipulation methods, and toxicological outcomes associated with ADF opioid abuse, and to develop simple in vitro tools for evaluating non-intended uses of ADFs.
Methodology:
Microfluidic channels with narrowed flow regions were designed to generate isolated high shear blood flow for comparison to a previously developed needle model. Different PEO formulations were introduced into blood and flowed through the channels. The blood flow rate and channel dimensions were varied to visualize and quantify thrombus formation. Hemolysis and clot size were measured to correlate with hematotoxicity and aberrant thrombosis.
Results:
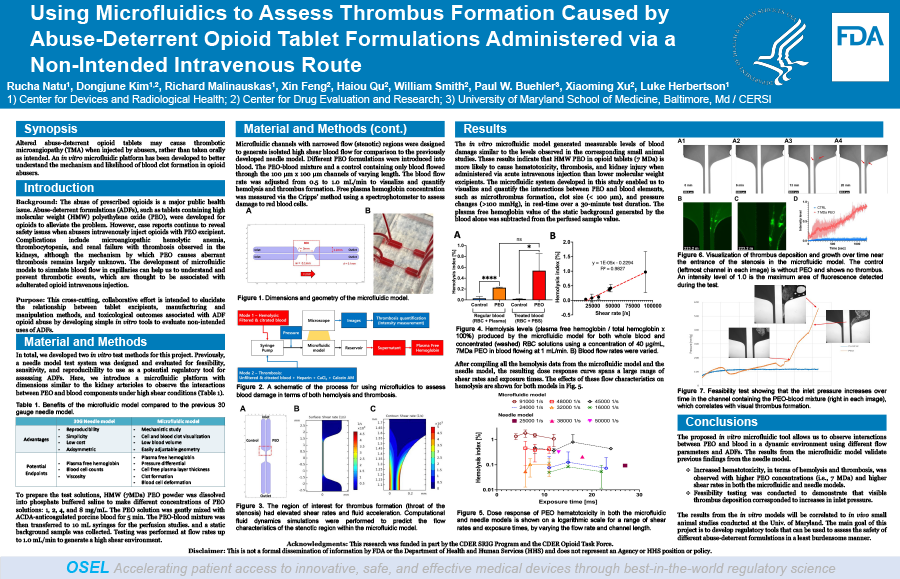
The in vitro microfluidic model generated measurable levels of blood damage which corresponded to small animal studies, confirming that HMW PEO in opioid tablets (> 1 MDa) is more likely to cause hematotoxicity, thrombosis, and kidney injury when administered via acute intravenous injection. The microfluidic system developed in this study had the added benefit of being able to visualize and quantify the interactions between PEO and blood elements, such as microthrombus formation, clot size (< 100 µm), and pressure changes (>100 mmHg), in real-time during the 30-minute test.
Conclusion:
The in vitro microfluidic tool provides us with insight into the PEO-blood interactions in a dynamic environment using different flow parameters and ADFs. The results from the microfluidic model validate previous findings from the needle model and small animal studies.