2023 FDA Science Forum
Claims-based Study of Transfusion-Related Acute Lung Injury (TRALI) Among Inpatient U.S. Medicare Beneficiaries Ages 65 and Older, 2007-2021
- Authors:
- Center:
-
Contributing OfficeCenter for Biologics Evaluation and Research
Abstract
Background:
TRALI is a leading cause of transfusion-related fatalities presenting as respiratory distress with non-cardiogenic pulmonary edema.
Purpose:
To assess TRALI occurrence, severity, and potential risk factors among inpatient Medicare beneficiaries, ages 65+, transfused during 2007-2021.
Methodology:
This is a hypothesis-generating study that utilized large Medicare databases, with transfusions identified by recorded procedure and revenue center codes, and TRALI by diagnosis codes. Unadjusted TRALI rates per 100,000 inpatient transfusion stays were evaluated by demographic and transfusion characteristics. Severity measures included inpatient mortality, mechanical ventilation, length of stay (LOS), and Charlson Comorbidity Index (CCI) score. Fisher’s exact tests compared rates and Cochran-Armitage tests ascertained trends by year, age, and units.
Results:
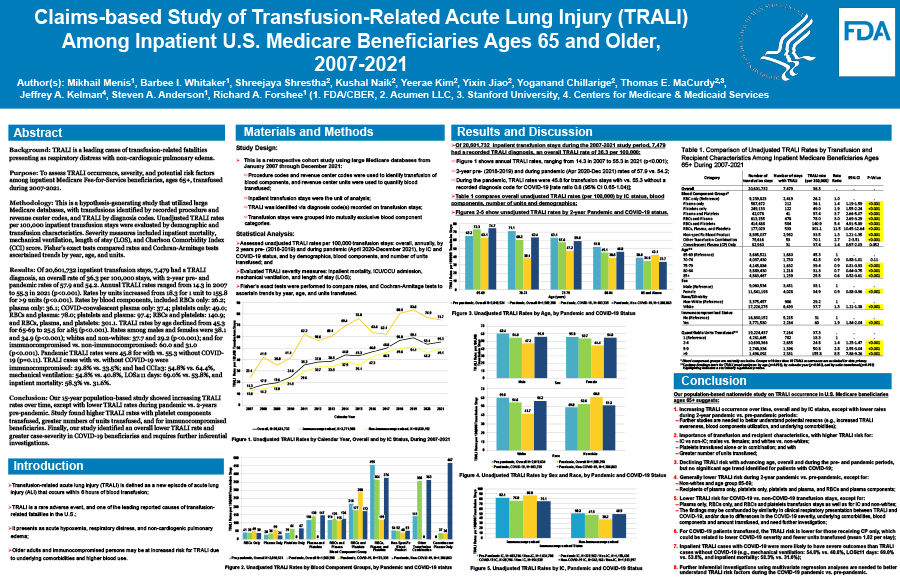
Of 20,601,732 inpatient transfusion stays, 7,479 had a TRALI diagnosis, an overall rate of 36.3, with 2-year pre- and pandemic rates of 57.9 and 54.2. Annual TRALI rates ranged from 14.3 in 2007 to 55.3 in 2021 (p<0.001). Rates by units increased from 18.3 for 1 unit to 155.8 for >9 units (p<0.001). Rates by blood components, included RBCs only: 26.2; plasma only: 36.1; COVID-convalescent plasma only: 37.4; platelets only: 49.0; RBCs and plasma: 78.0; platelets and plasma: 97.4; RBCs and platelets: 140.9; and RBCs, plasma, and platelets: 301.1. TRALI rates by age declined from 45.3 for 65-69 to 25.5 for ≥85 (p<0.001). Rates among males and females were 38.1 and 34.9 (p<0.001); whites and non-whites: 37.7 and 29.2 (p<0.001); and for immunocompromised vs. non-immunocompromised: 60.0 and 31.0 (p<0.001). Pandemic TRALI rates were 45.8 for with vs. 55.3 without COVID-19 (p=0.11). TRALI cases with vs. without COVID-19 were immunocompromised: 29.8% vs. 33.5%; and had CCI≥3: 54.8% vs. 64.4%, mechanical ventilation: 54.8% vs. 40.8%, LOS≥11 days: 69.0% vs. 53.8%, and inpatient mortality: 58.3% vs. 31.6%.
Conclusion:
Our 15-year population-based study showed increasing TRALI rates over time, except with lower TRALI rates during pandemic vs. 2-years pre-pandemic. Study found higher TRALI rates with platelet components transfused, greater numbers of units transfused, and for immunocompromised beneficiaries. Finally, our study identified an overall lower TRALI rate and greater case-severity in COVID-19 beneficiaries and requires further inferential investigations.