Testimony | In Person
Event Title
The Path Forward: A Federal Perspective on the COVID-19 Response
July 20, 2021
- Testimony of
-
Janet Woodcock, M.D.
- Before the
Introduction
Chair Murray, Ranking Member Burr, distinguished members of the Committee, I am Dr. Janet Woodcock, Acting Commissioner of the U.S. Food and Drug Administration (FDA or the Agency). Thank you for the opportunity to testify before you today to describe FDA’s coronavirus disease 2019 (COVID-19) response efforts. All of our efforts are in close coordination and collaboration with our partners, both within the Department of Health and Human Services (HHS) and across the Federal government, to help ensure the development, authorization, licensure, and availability of critical, safe, and effective medical products to address the COVID-19 public health emergency.
I want to note at the outset that this is just a snapshot of some of our recent work and is in the context of efforts across the Agency to address this pandemic. There are thousands of FDA employees who have been working non-stop for the past year-and-a-half. I want to commend and recognize their efforts and thank them for their service.
From the beginning of this public health emergency, FDA has taken an active leadership role in the all-of-government response to the COVID-19 pandemic, inspired by the resiliency of the American people and our great innovators. FDA stood up an internal cross-agency group that continues to ensure we are doing everything possible to protect the American public, help ensure the safety, efficacy, and quality of FDA-regulated medical products, and provide the industries we regulate with the guidance and tools to do the same. We continue to focus on facilitating the development and availability of medical countermeasures to diagnose, treat, and prevent COVID-19, surveilling the medical product and food supply chains for potential shortages or disruptions, and helping to mitigate such impacts, as necessary to protect the public health.
Biologics and Vaccines
FDA’s Center for Biologics Evaluation and Research (CBER) uses every tool available to help patients access promising biological products while facilitating research to evaluate their safety and efficacy as well as manufacturing efforts.
CBER is working on multiple fronts to address the COVID-19 pandemic, including:
- Expediting clinical trials for vaccines and certain therapeutic biological products that hold promise to prevent or treat COVID-19 by providing timely interactions, scientific advice, and recommendations for specific sponsors, and generally through guidance documents;
- Supporting product development and facilitating the scaling up of manufacturing capacity for high priority products to treat COVID-19;
- Expediting the review of Emergency Use Authorization (EUA) requests and Biologics License Applications (BLAs) for critical medical products to address COVID-19;
- Helping to ensure an adequate and safe blood supply; and
- Providing information to healthcare providers and researchers to help them submit expanded access IND requests to permit the use of investigational products for patients with COVID-19.
Through our transparent scientific review process, FDA has issued EUAs for three COVID-19 vaccines. In doing so, we have relied upon the Agency’s rigorous standards for safety, effectiveness, and manufacturing quality. Development of a vaccine generally proceeds sequentially through the various stages of clinical development; ordinarily this process minimizes scientific and financial risk for the manufacturer. Manufacturing scale-up only takes place when the data support the safety and effectiveness of a vaccine and it is on track for regulatory approval. These three COVID-19 vaccines were developed without cutting corners or sacrificing our standards. Intensive interactions between FDA and manufacturers minimized the time between different studies in the clinical development process; allowed seamless movement throughout the different phases of clinical trials; and simultaneously facilitated manufacturers proceeding with manufacturing scale-up before it was clear whether the safety and effectiveness data for a vaccine would support EUA.
For the three vaccines authorized to date, our EUA process not only included a thorough evaluation of the data by the Agency’s career staff, but also included input from independent scientific and public health experts through our public advisory committee meetings. Throughout this process, FDA took additional steps to facilitate transparency, such as posting sponsor and FDA briefing documents and key decisional memoranda.
The three authorizations make available COVID-19 vaccines in the United States that have shown clear and compelling efficacy in large, well-designed phase 3 trials. These vaccines have met rigorous standards for safety and effectiveness to support EUA and are helping us in the fight against this pandemic. All the COVID-19 vaccines that FDA has authorized for emergency use are at least 50 percent effective compared to placebo in preventing COVID-19, which is the expectation we conveyed in our June 2020 guidance document, Development and Licensure of Vaccines to Prevent COVID-19.1 A vaccine with at least 50 percent efficacy, we noted, would have a significant impact on disease, both at the individual and societal level.
As part of our continued efforts to be transparent and educate the public, we have a wealth of information on our website about the authorized COVID-19 vaccines. The information includes fact sheets for healthcare providers (vaccination providers) and vaccine recipients and caregivers, with important information such as dosing instructions; information about the benefits and risks of each authorized vaccine; and topical Questions and Answers developed by FDA for each authorized vaccine.2
It is also important to highlight that, as part of each EUA, we are requiring the manufacturers and vaccination providers to report serious adverse events, cases of Multisystem Inflammatory Syndrome (MIS), and cases of COVID-19 that result in hospitalization or death to the Vaccine Adverse Event Reporting System (VAERS), a national vaccine safety surveillance program jointly run by FDA and the Centers for Disease Control and Prevention (CDC).
These surveillance efforts have led the Agency to take steps to proactively address emerging safety signals. In April, out of an abundance of caution, FDA and CDC recommended a pause in the use of the Janssen COVID-19 vaccine while we investigated reports of thrombosis with thrombocytopenia syndrome. Later that month, after careful evaluation of the data, FDA announced revisions to the vaccine recipient fact sheet to include information about the risk of thrombosis with thrombocytopenia, and the vaccination provider fact sheet to include a warning about the risk of thrombosis with thrombocytopenia syndrome. We concluded that the available data suggest that the chance of this serious adverse event occurring is very low. FDA and CDC determined that the recommended pause regarding the use of the Janssen COVID-19 vaccine in the U.S. should be lifted and use of the vaccine should resume. As with all of the COVID-19 vaccines, we continue to closely monitor the safety of the Janssen COVID-19 Vaccine.
On June 25, FDA announced revisions to the vaccine recipient and caregivers and vaccination provider fact sheets for the Moderna and Pfizer-BioNTech COVID-19 vaccines regarding the suggested increased risks of myocarditis and pericarditis following vaccination. The chance of these adverse events occurring following administration of either the Moderna or Pfizer-BioNTech COVID-19 vaccine appears to be very low, but the level of potential risk due to vaccination is still under investigation. FDA and CDC are monitoring the reports, collecting more information, and will follow up to assess longer-term outcomes over several months.
On July 12, FDA announced revisions to the vaccine recipient and caregivers and vaccination providers fact sheets for the Janssen COVID-19 vaccine regarding a suggested increased risk of Guillain-Barré syndrome during the 42 days following vaccination. The chance of this occurring following vaccination appears to be very low.
At this time, data are not yet available to make a determination about how long these authorized vaccines will provide protection, nor are we certain that the vaccines prevent transmission of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) from person to person. Additionally, although we do not yet know the full range of SARS-CoV-2 variants that each of the authorized vaccines will protect against, there is evidence that the current vaccines protect against disease caused by variants circulating in the United States.
Finally, manufacturers whose COVID-19 vaccines have been authorized for emergency use are expected to continue their clinical trials in order to obtain additional safety and effectiveness information and pursue licensure (approval).
Having three vaccines authorized to date that meet FDA’s expectations for safety and effectiveness only one year after the declaration of the COVID-19 pandemic is a tremendous achievement and a testament to the dedication of developers and FDA’s career scientists and physicians. We are highly engaged in ensuring that all COVID-19 vaccines meet the high quality that Americans expect and deserve and are also actively engaged in ensuring the safety of these vaccines following deployment. FDA is also working with international partners as part of multinational efforts to end this global pandemic. We have provided guidance and technical assistance, and continue to share information as we evaluate and release vaccine doses for use in other countries. The Agency is very proud of these efforts, and we believe that the vaccines will help bring this pandemic to an end.
Therapeutics
Since the beginning of the COVID-19 pandemic, FDA has been working tirelessly to facilitate the development and availability of therapeutics for use by patients, physicians, and health systems as expeditiously and safely as possible. FDA has also accelerated the development and publication of guidance and other information for industry and researchers on developing COVID-19-related treatments. Further, on March 31, 2020, FDA announced the creation of an emergency review and development program for possible therapies for COVID-19, the Coronavirus Treatment Acceleration Program, or “CTAP.” The primary goal of CTAP is to help accelerate the development of therapeutics for patients and consumers. The Agency has supported the program by reassigning staff and working continuously to review requests from companies, scientists, and doctors who are working to develop therapies. Under CTAP, FDA is using every available authority and regulatory flexibility to facilitate the development of safe and effective products to treat patients with COVID-19. As of June 30, 2021, there are more than 630 drug development programs in planning stages and the Agency has reviewed more than 460 trials of potential therapies for COVID-19. These include antivirals, immunodulators, neutralizing antibodies, cell and gene therapies, and combinations of these products. The diversity of therapeutic approaches being investigated is important because it rapidly expands our understanding of the effect of different categories of potential treatments.
FDA has approved one drug to treat COVID-19 and eleven therapeutics are currently authorized for emergency use. Our goal is to be as transparent as possible about the scientific basis for recommending that a drug or biological product be authorized for emergency use under section 564 of the Federal Food, Drug and Cosmetic Act (21 U.S.C. 360bbb-3) or for recommending that an EUA be revised or revoked.
FDA also continues to work closely with manufacturers to mitigate and prevent shortages as
the COVID-19 pandemic evolves. For example, the Agency has issued three EUAs to authorize the emergency use of certain therapeutic products intended to treat serious or life-threatening diseases or conditions (e.g., Acute Kidney Injury, Acute Respiratory Distress Syndrome) caused by COVID-19 after determining that the FDA-approved alternatives to these products were not available in sufficient quantities to fully meet the emergency need. This has helped to alleviate shortages of some therapies that are essential for the care of critically ill COVID-19 patients. FDA is also working with manufacturers to increase supplies to meet current demand by expediting review of applications. In addition, the Agency has prioritized the review of generic drug applications for potential treatments and supportive therapies for patients with COVID-19, such as antibiotics, sedatives used in ventilated patients, anticoagulants, and pulmonary medications. In June 2021, FDA reached a milestone of approving 1,000 original and supplemental generic drug applications since the start of the pandemic to help in the treatment of patients with COVID-19. This supports FDA’s everyday mission of improving access to safe, effective, high-quality treatment options, especially during the COVID-19 pandemic.
Medical Devices
The need for medical devices to respond to the COVID-19 pandemic has far exceeded what we experienced in any prior Public Health Emergency (PHE). The first EUAs issued for the COVID-19 PHE were for medical devices, and the volume of EUA requests quickly surpassed (by two orders of magnitude) that of any prior PHE or other situation. Further, the emergency use requests included submissions for devices that CDRH had never received EUA requests for during prior PHEs. This included ventilators and novel devices such as continuous renal replacement therapy devices. Since the start of the pandemic, FDA has issued EUAs or granted full marketing authorization to almost 1,500 medical devices for COVID-19-related uses. In addition, FDA rigorously monitored safety signals and medical device reports using the information to publish 21 letters to healthcare providers and seven safety communications, and FDA completed other pivotal work activities such as addressing supply chain shortages and counterfeit products related to COVID-19.
Diagnostic tests are the first line of defense in an outbreak, and FDA plays an important role to ensure they work through EUA review. The EUA pathway expedites access to accurate diagnostic tests during emergencies, when information gaps and false results may adversely affect individual patient care and public health decision making. EUAs enable molecular diagnostic tests to be developed, validated, authorized, and deployed within weeks rather than several months to over a year, as is typical for test development and traditional premarket submissions. The Agency has employed its EUA authorities to facilitate availability of tests in each PHE or threat situation since 2009, when the Secretary of HHS declared that circumstances exist justifying the authorization of emergency use of in vitro diagnostics. In PHEs, FDA is generally open to receiving and reviewing EUA request for tests from any developer, including commercial kit manufacturers and laboratories.
FDA sought to facilitate COVID-19 test evaluation and authorization through the development and availability of templates. The templates provide recommendations for test validation and a fill-in-the-blank form to streamline the paperwork and make it easier for developers to provide information in support of a request for emergency use authorization. Since providing the first template in January 2020, FDA has been in daily contact with test developers to answer questions and help them through the EUA process. This has proved to be a helpful tool for many. FDA has now made nine templates available for a variety of test types. As of July 13, 2021, these nine templates have received 510,725 hits from those visiting FDA’s website. FDA also supported test developers through establishment of a dedicated mailbox, 24-7 toll-free hotline that ran until July 2020, the posting of over 100 frequently asked questions on our website, and by hosting weekly virtual town halls for test developers. The Agency has worked with over 1,000 test developers since January 2020.
Since early 2020, FDA has adopted agile, interactive, and innovative approaches to EUA review for all types of devices. For example, FDA developed the umbrella EUA approach to efficiently authorize multiple devices of the same type meeting the same criteria. The Agency has also issued 28 guidance documents (including 17 revisions) outlining policies to help expand the availability of medical devices needed in response to COVID-19. For example, developers of certain tests offered their tests, upon validation and notification to FDA prior, to issuance of an EUA during Agency review of the EUA request. Further, FDA made several improvements to our EUA review processes to make the most efficient use of our resources, including establishing a front-end triage process to identify devices that would have the greatest impact on the public health. These improvements incorporate the latest information on device availability and shortages, prioritizing novel or critical devices not yet available on the market or those that would address significant device shortages.
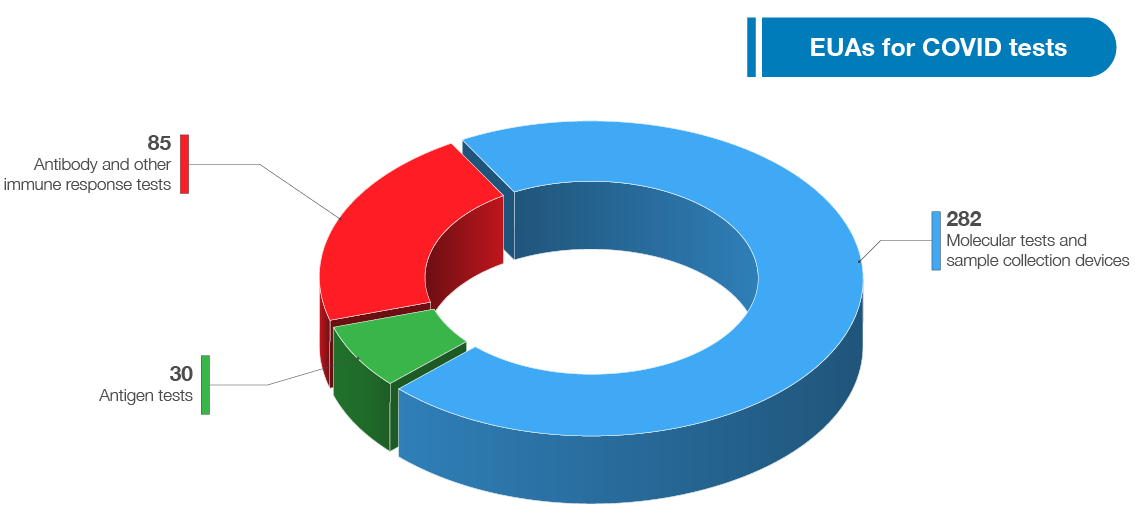
As of July 13, 2021, FDA has authorized 397 tests and sample collection devices for SARS-CoV-2. As noted in the graphic below, these include 282 molecular tests and sample collection devices, 85 antibody and other immune response tests, and 30 antigen tests. Among these are 11 diagnostic tests that can be run at home (three molecular and eight antigen tests), seven of which do not require a prescription. We have also authorized 18 tests for serial screening programs (11 antigen and seven molecular). The volume and variety of available tests is a testament to FDA’s support of innovative test design and our commitment to public health.
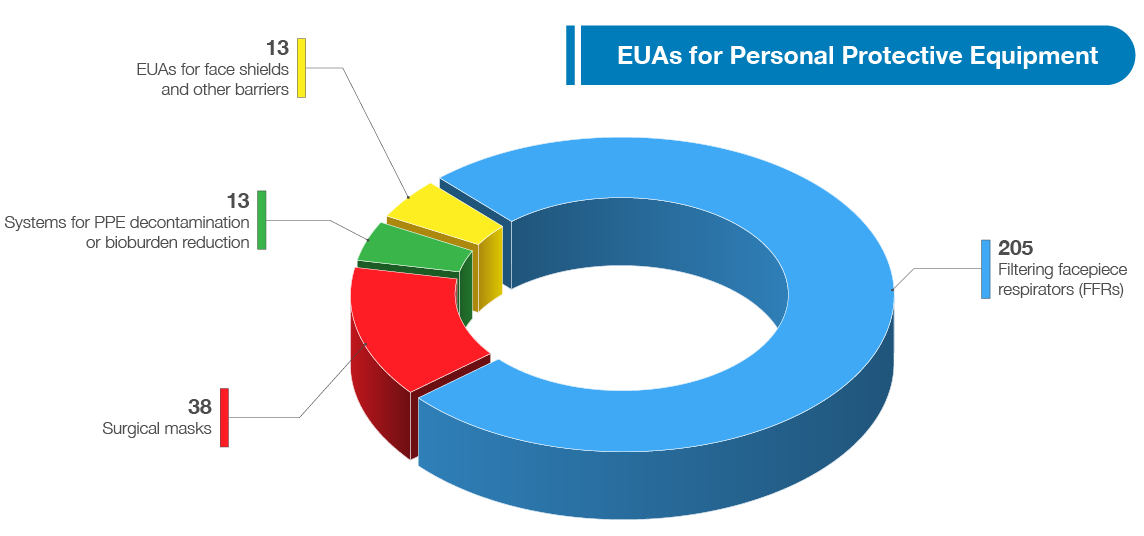
FDA has authorized a wide variety of other medical devices for use in combating the pandemic, including a wide range of personal protective equipment (PPE), ventilators, and other therapeutic devices. As of July 13, 2021, FDA has authorized 270 PPE devices including 39 surgical masks, and has authorized 205 filtering facepiece respirators (FFRs), 13 systems for PPE decontamination or bioburden reduction at the time there was a need for these types of devices due to PPE shortages,3 and 13 EUAs for face shields and other barriers intended to protect the user from bodily fluids, liquid splashes, or potentially infectious materials (see related graphic below). In addition to granting EUAs, FDA has also cleared, through its premarket notification pathway, over 250 PPE 510(k)s.
FDA recognizes that medical devices, particularly tests, will continue to play an important role in the next phase of the pandemic response. The Agency is continuing to monitor its policies, the marketplace, and national needs, and will continue to adapt as the circumstances of the evolving pandemic warrant.
Human and Animal Food
Food security is national security. Thus, throughout the pandemic, FDA has worked with federal, state, and local partners, as well as industry, to help ensure a safe and adequate food supply for both people and animals.
While SARS-CoV-2 is not transmitted by food, some components of the food system experienced challenges and supply chain imbalances, particularly at the outset of the pandemic. Overall, food production and manufacturing in the U.S. has remained resilient. We continue to monitor the food supply chain systems closely to efficiently and promptly identify mitigation strategies when necessary. Early on, the pandemic caused a significant shift in where consumers were buying food. We took steps to provide temporary guidance to provide flexibility in packaging and labeling requirements to help industry redirect products manufactured for food service and institutional use to retail grocery stores, or if needed to the animal food industry so the food does not go to waste.
FDA also recognizes that food supply chain continuity and worker safety are two sides of the same coin. Thus, a robust food supply is dependent on the safety and health of the nation’s food and agricultural workforce. Along with our federal, state and local partners, we have provided best practices for food and agricultural workers, industry, and consumers on how to stay safe, and help ensure the continuity of operations in the food and agriculture critical infrastructure sector during the pandemic and now as restaurants and other retail establishments resume regular operations.
In response to the pandemic, FDA’s Office of Food Policy and Response, Center for Food Safety and Applied Nutrition, Office of Regulatory Affairs, and Center for Veterinary Medicine developed 21 Forward, a food supply chain data management tool, to help identify where risks for interruptions in the continuity of the food supply due to COVID-19 transmission among workers may be greatest. As part of 21 Forward, FDA also conducted targeted outreach to the food industry to offer additional resources and technical assistance in addressing challenges.
In collaboration with HHS, CDC, and US Department of Agriculture (USDA), data from 21 Forward have been made available to assist states with their vaccine distribution efforts for workers in the food and agriculture sectors, including migratory and seasonal agricultural workers.
FDA’s Coordinated Outbreak Response and Evaluation team has been working throughout the pandemic, is fully staffed, and on the job looking for signs of foodborne illness outbreaks and initiating responses as needed. FDA’s Center for Veterinary Medicine is also monitoring the animal food supply and initiating needed responses, working closely with other veterinary diagnostic laboratories in its Veterinary Laboratory Investigation and Response Network (VET-LIRN). In terms of inspectional work, FDA investigators continue to conduct mission-critical inspections domestically and abroad, including inspections and investigations in response to foodborne outbreaks during the pandemic. FDA transitioned to standard operations for domestic surveillance inspections in July 2021. Additionally, our import investigators and laboratory analysts continue to work on-site by:
- Staffing our ports of entry, helping to ensure the efficient distribution and safety of the nation’s imported food supply; and
- Conducting examinations, sample collections, and laboratory analyses of imported and domestic food to ensure the safety of our nation’s food supply.
FDA continues to screen every line of every shipment of imported food entering the United States utilizing our Predictive Risk-Based Evaluation for Dynamic Import Compliance Targeting (PREDICT) tool. We adjusted the algorithm in PREDICT to place increased scrutiny on shipments from facilities where foreign inspections have been postponed. FDA has made greater use of our Foreign Supplier Verification Program (FSVP) regulation to oversee compliance with FDA Food Safety Modernization Act (FSMA) requirements. The shift to remote FSVP inspections, along with other tools utilized by the foods program, has been critical to ensuring the safety of human and animal food from foreign suppliers during the COVID-19 pandemic. Since March 26, 2020, FDA has conducted 1,888 FSVP inspections. Since March 2020, FDA has refused approximately 8,469 lines of imported food products. FDA will continue to target and refuse human and animal foods that are unsafe, misbranded, or may cause a serious health concern for the public.
FDA continues to closely monitor the overall safety of the nation’s food supply, in collaboration with CDC, USDA, U.S. Customs and Border Protection (CBP) and our state and local partners, to protect consumers from foods contaminated with pathogens.
One year ago, FDA announced the New Era of Smarter Food Safety Blueprint outlining the Agency’s plans over the next decade to create a more digital, traceable, and safer food system. We have learned from our response as an Agency to the pandemic that there is an accelerated need for certain goals in this blueprint, especially those involving supply chain continuity and resilience, modernized inspectional approaches, and strengthening food safety infrastructures with regulatory partners.
Inspections, Compliance, and Protecting the Medical Supply Chain
Similar to their work protecting the food supply, import investigators have been on site protecting the medical supply chain at our ports of entry, courier facilities, and the international mail facilities (IMFs) throughout the pandemic. Through continued vigilance, FDA has prevented unsafe and unauthorized pharmaceuticals and other medical products from entering the country. Since March 2020, with the cooperation of and in coordination with CBP, FDA has received and destroyed almost 60,000 products, totaling over 11,093,868 capsules, pieces, and tablets of illegal or unapproved drugs.
Since March 2020, FDA has refused approximately 94,725 lines of imported violative medical products. We have maintained the same level of pre-pandemic screening for imported products. However, FDA has focused examinations on COVID-19 relief supplies to ensure compliant products are expedited while maintaining our commitment to refusing imported medical products that are unsafe, misbranded, unapproved, counterfeit, or may cause serious illness or injury to the public. In fact, our import and domestic officers have evaluated donations of shipments destined for the Federal Emergency Management Agency (FEMA) and met the first vaccines (Pfizer Belgium) on their arrival into the United States in December 2020 to ensure proper transport, storage, and reconciliation of products. Our officers also assisted with expediting the importation of other compliant vaccine-related shipments.
Despite pausing domestic and foreign surveillance inspections in March 2020 to safeguard the health and well-being of our staff, as well as employees at facilities we inspect, our investigators continued to conduct mission-critical inspections both domestically and abroad to ensure FDA-regulated industries were meeting applicable FDA requirements. In July 2020, FDA resumed prioritized domestic inspections. To arm our investigators with the most reliable and accurate information, FDA developed a rating system to assist in determining when and where it was safest to conduct prioritized domestic inspections.
On May 5, 2021, FDA issued a report titled, “Resiliency Roadmap for FDA Inspectional Oversight,” outlining the Agency’s inspectional activities during the COVID-19 pandemic and its detailed plan to move toward a more consistent state of operations, including FDA’s priorities related to this work going forward.
The report outlines inspections that the Agency was unable to complete during the past year due to travel restrictions or inability to ensure the safety of our workforce or the workforces within the industries the Agency regulates. The report also outlines the number of mission-critical inspections FDA completed during that time, such as inspections of facilities for which there was a drug shortage, inspections needed for the approval of novel drugs or drugs related to the potential treatment of COVID-19, support of pre-market and pre-license applications, and response to foodborne disease outbreaks or other food safety risks such as food contaminated with pathogens.
Of note:
- From March 2020 through March 2021, FDA conducted a total of 821 mission-critical inspections, including 29 in foreign countries.
- Additionally, the Agency conducted a total of 777 prioritized domestic inspections since resumption of that work in July 2020.
- Of the more than 13,500 applications for medical product approval or authorization received since March 2020, only approximately 68 applications have been delayed due to the inability to conduct inspections — and a majority of these applications are not deemed mission-critical.
Additionally, the Resiliency Roadmap Report outlines FDA’s continued, successful use of alternative tools and approaches where inspections were or are not currently feasible, including remote interactive evaluations (e.g., remote livestreaming video of operations, teleconferences, or screen sharing), making record requests to regulated establishments, and leveraging information from trusted regulatory partners. For example, FDA made over 1,300 record requests to human and animal drug and biological product manufacturers, to support on-time regulatory decision actions. In addition, since March 2020, FDA has added products from 18 firms to import alerts as subject to detention without physical examination, based on records requests in advance or in lieu of inspection that FDA submitted pursuant to section 704(a)(4) of the FD&C Act.
Notably, FDA’s bioresearch monitoring program staff have conducted more than 130 remote interactive evaluations that were directly used for application decisions.4 The new tool was incentivized for and supported by industry and continues to provide the Agency with valuable information to assist with risk-based targeting for inspections. FDA recognizes that remote approaches do not replace inspections, and that there are situations where only an inspection is appropriate based on risk and history of compliance with FDA regulations.
The Resiliency Roadmap Report further outlines the ongoing steps the Agency is taking to resume standard operational levels of inspection activities, including how it intends to prioritize domestic and foreign inspections that were not performed during the pandemic. The plan highlights a variety of possible scenarios given the continued uncertainty of the trajectory of the ongoing COVID-19 pandemic. On July 1, FDA activated the base-case scenario (COVID response continues on current trend) to transition to standard operations for domestic inspections and other operational work, as detailed in the report. Inspections considered critical to FDA’s mission will remain the primary focus. When planning routine surveillance inspections, the Agency will prioritize higher-risk establishments. This means that postponed inspections will be prioritized based on risk and conducted over a longer period of time, ultimately increasing the amount of time between inspections of certain lower-risk facilities in order to focus on products that present the greatest risk to public health.
The Agency will also soon begin a multi-year modernization effort to further transform our data enterprise platforms and cross-program interoperability infrastructure to better support innovation related to its regulatory oversight role. This includes adopting technology to support regulatory assessments to improve our remote receipt, review, and analysis of industry data and records, and improve remote interactions with industry entities to be easier, more efficient, more consistent, and more secure. This modernization effort will include a review of inspectional approaches using next-generation assessment technologies and improvements. FDA is also establishing an Agency-wide Inspectional Affairs Council that will provide for coordination of inspection approaches and assessment processes. The Agency intends to share more information on these efforts as this work progresses. FDA will continue to leverage and maximize every available tool and resource to meet its inspectional responsibilities, while achieving optimal public health outcomes.
Compliance and Enforcement
FDA exercises its regulatory authority by, among other things, issuing warning letters and pursuing civil and criminal actions against firms and individuals who do not comply with regulatory requirements, including those selling unapproved products with false or misleading claims that the products prevent, treat, mitigate, diagnose, or cure COVID-19. In March 2020, FDA launched Operation Quack Hack, which leverages Agency expertise and advanced analytics to protect consumers from fraudulent medical products, including unproven cures, illegitimate test kits, and substandard or counterfeit respirators. FDA has sent thousands of abuse complaints to domain name registrars and internet marketplaces. The Agency also has sent more than 241 warning letters to sellers of unproven COVID-19 products. Working with the Department of Justice (DOJ), FDA has sought and obtained preliminary injunctions that require defendants to halt the sale of fraudulent products claiming to treat or prevent COVID-19, including one product, “Miracle Mineral Solution,” that, when used as directed, is equivalent to industrial bleach.
In addition, FDA’s Office of Criminal Investigations (OCI), working with other federal and local law enforcement agencies, investigated a hospital pharmacist who tampered with COVID-19 vaccine doses at a Wisconsin hospital where he worked. On two successive overnight shifts at the hospital in late December 2020, the pharmacist purposefully removed a box of COVID-19 vaccine vials manufactured by Moderna—which must be stored at specific temperatures for specific time periods to remain viable—from the hospital’s refrigeration unit intending to render the vaccines inert and no longer effective. The pharmacist acknowledged that after leaving the vaccines out for several hours each night, he returned them to the refrigerator to be used in the hospital’s vaccine clinic the following day. Before the full extent of his conduct was discovered, 57 people received doses of the vaccine from these vials. In January 2021, the pharmacist pled guilty to two counts of attempting to tamper with consumer products with reckless disregard for the risk that another person will be placed in danger of death or bodily injury. He has been sentenced to three years imprisonment, followed by three years of supervised release, and he must pay approximately $83,800 in restitution to the hospital.
In addition, FDA investigators remain on the front lines at ports of entry, quickly examining, reviewing, and sampling import entries, and refusing admission where appropriate. We protect the supply chain in two equally critical ways, by helping to ensure that 1) safe products are coming in; and 2) illegal, dangerous, and fraudulent products do not get into the country. These efforts include partnering with CBP in establishing satellite laboratories at selected IMFs with scientists using state-of-the-art screening tools to rapidly identify unapproved, counterfeit and illicit products.
In March 2020, OCI, with the help of domestic law enforcement partners and foreign counterparts in the United Kingdom, led the investigation of fraudulent COVID-19 “treatment kits” that were falsely declared as “water treatment.” Import examination of these shipments found misbranded “kits” intended to treat SARS-CoV-2. As a result of this investigation, a British national was charged and arrested for shipping mislabeled and unapproved products. Subsequently, in April 2020, FDA intercepted a bulk shipment of hydroxychloroquine coming from China going to a physician in California. The physician was thereafter charged with mail fraud and making a false statement stemming from the allegations that he smuggled hydroxychloroquine from China to make his own pills and concealed the shipment from CBP by mis-declaring it as yam extract. In May 2020, FDA worked with CBP to intercept several shipments of counterfeit facemasks, with the result that they were refused and destroyed before getting into U.S. commerce.
More recently, FDA has taken steps to address hand sanitizer products that pose safety concerns, such as products that do not meet the required ethanol or isopropanol levels, or that contain or may contain toxic ingredients like methanol or 1-propanol. Regarding the latter, substantial methanol exposure can result in nausea, vomiting, headache, blurred vision, permanent blindness, seizures, coma, permanent damage to the nervous system or death. Ingesting 1-propanol can cause central nervous system depression, which can result in death. FDA has tested several hundred products using field-based and laboratory-based tools, found more than a hundred violative products, issued warnings to consumers not to use contaminated hand sanitizers, and has taken steps to help ensure that these dangerous or subpotent products do not enter domestic commerce. FDA has coordinated with CBP to identify such products, and we have listed products made by more than 40 manufacturers on import alert. FDA also placed all alcohol-based hand sanitizers from Mexico on a countrywide import alert to help stop products from entering the United States that appear to be in violation until the Agency is able to review the products. That action marked the first time the FDA has issued a countrywide import alert for any category of drug product.
Medical Product Supply Chain
FDA monitors and responds to worldwide demand and supply chain disruptions for medical products caused by the COVID-19 pandemic. We work closely with manufacturers to help ensure they continue to notify the Agency of any permanent discontinuance or interruption of drug (human and animal), biological product, and device manufacturing in a timely manner and, as noted in FDA’s FY 2022 budget, we are working to better position the Agency and our health care system to assure a strong domestic supply chain in future emergencies.5
In addition to our usual communication with drug manufacturers, we work closely with healthcare and pharmacy systems, hospitals, providers, and others on the frontlines of COVID-19 patient care to identify current or emerging regional shortages of critical care drugs used to treat COVID-19.
FDA understands the significant impact shortages can have on patient care and is doing everything within our authorities to help prevent and alleviate disruptions. When we identify a shortage, we react swiftly to mitigate the impact to U.S. patients and health care professionals, and quickly share that information with the public. For example, we issued temporary policies for outsourcing facilities registered with FDA and pharmacists in state-licensed pharmacies or federal facilities, regarding the compounding of certain drugs used to treat hospitalized patients with COVID-19 when approved drugs are not available. The Agency has also published guidance to help applicants and manufacturers provide FDA with timely and informative notifications about changes in the production of certain drugs (including animal drugs) and human biological products, and urging the submission of these notifications, which may assist in our efforts to prevent or mitigate shortages of such products.
The Agency quickly identified the need to help ensure widespread access to hand sanitizers as demand spiked, while also continuing our mission to ensure these products are not contaminated by removing adulterated products from the market. FDA has published and continues to update three guidance documents designed to help facilitate the production of alcohol-based hand sanitizer in non-traditional settings such as pharmacies or distilleries. The Agency has launched several enforcement initiatives and import alerts to help stop adulterated and subpotent hand sanitizer products from getting into U.S. distribution channels.
Our experience with COVID-19 demonstrates that a strong domestic supply chain depends on a resilient supply chain for medical devices as well. Indeed, multiple entities across the public and private sector have important parts to play in strengthening the domestic medical device supply chain. FDA can play a critical role in identifying and preventing shortages for devices, because the Agency not only reviews and authorizes these products, but also has unique, collaborative relationships that allow direct engagement with device manufacturers, patients, distributors, healthcare organizations and other stakeholders. Even before the pandemic hit the United States, there were already problems in the supply chain due to demand for devices in other nations where COVID-19 was already prevalent. As a result, FDA began shortage mitigation activities for medical devices in January 2020 before the PHE was declared in the U.S., and months before a pandemic was declared worldwide. The Agency took several actions to rapidly respond to supply chain needs, including reassigning 130 staff to perform shortages work across CDRH and contacting over 1,000 manufacturing facilities in 12 countries in just a few weeks’ time to get as much information as possible about critical devices.
In addition, FDA has conducted horizon scanning to assess demand for devices needed to respond to the pandemic, including PPE, ventilators, diagnostic supplies, infusion pumps, and non-contact infrared thermometers; and established a rapid response team, working with field personnel to address fraudulent imports. The Agency has likewise worked to prevent and mitigate shortages of testing supplies. For example, FDA collaborated with U.S. Cotton, one of the world’s largest manufacturers of cotton swabs, to develop and produce a polyester-based swab for testing. FDA also collaborated with laboratories and clinical investigators validating potential alternative sources of control materials, transport media, and swabs. As individual developers validated these alternative components, FDA requested their permission to share their findings publicly so that others could benefit, and we posted these alternatives on our website. In this way, FDA has been serving as a clearinghouse for scientific information that the entire community can leverage to mitigate shortages and increase testing capacity. FDA continues to post this information on a rolling basis on an FAQ website so that labs have access to the latest information regarding alternative controls, transport media, extraction, instruments, and swabs.
Congress has acknowledged the importance of this work to our health care system, and we want to continue working with this committee and others to ensure FDA has the resources and authorities needed to ensure U.S. patients and health care providers have the products they need each day, and especially during public health emergencies.
Conclusion
FDA continues to advance its mission to protect and promote public health by ensuring the safety of human and animal food, and the safety and effectiveness of medical products. We take our public health mandate very seriously and will continue to work each day to end this pandemic. We continue to communicate with the American public and make regulatory decisions based on data and sound science. I look forward to continuing to work with the Committee on these efforts and thank you again for the opportunity to testify today.
- 1https://www.fda.gov/media/139638/download
- 2https://www.fda.gov/emergency-preparedness-and-response/coronavirus-disease-2019-covid-19/covid-19-frequently-asked-questions
- 3https://www.fda.gov/news-events/press-announcements/fda-brief-fda-revokes-emergency-use-authorizations-certain-respirators-and-decontamination-systems
- 4https://www.fda.gov/regulatory-information/search-fda-guidance-documents/remote-interactive-evaluations-drug-manufacturing-and-bioresearch-monitoring-facilities-during-covid
- 5https://www.fda.gov/media/149616/download