Testimony | In Person
Event Title
FDA User Fee Reauthorization: Ensuring Safe and Effective Drugs and Biologics
February 3, 2022
- Testimony of
-
Patrizia Cavazzoni,, M.D.
Director - Center for Drug Evaluation and Research
Director - Center for Drug Evaluation and Research ( April 2021 - January 2025 )
- Before the
Introduction
Chair Eshoo, Ranking Member Guthrie, and Members of the Subcommittee, thank you for the opportunity to testify today on the reauthorizations of the Prescription Drug User Fee Act (PDUFA), Generic Drug User Fee Amendments (GDUFA), and the Biosimilar User Fee Act (BsUFA) and the Food and Drug Administration’s (FDA, the Agency, or we) efforts to deliver timely access to safe and effective medications for all Americans. We appreciate the efforts of Congress and this Committee particularly in successfully reauthorizing these programs in previous cycles and look forward to continuing our partnership this year.
PDUFA
The PDUFAVII reauthorization proposal described below was submitted to Congress on January 12, 2022. The Administration looks forward to working with Congress on reauthorization of PDUFA to continue to speed the development and approval of vital drugs and biologics that are safe and effective.
The timely review of the safety and effectiveness of new drug applications (NDAs) and biologics license applications (BLAs) is central to FDA’s mission to protect and promote the public health – and PDUFA is essential to these efforts.
FDA is committed to scientific quality and integrity during its review process for marketing applications to ensure that the medications we approve are safe and effective for American patients. Before PDUFA’s enactment in 1992, the Agency lacked sufficient staff to perform timely reviews or develop procedures and standards to ensure a consistent and predictable premarket review process. As a result, Americans’ access to innovative, new medicines often lagged behind other countries.
The enactment of PDUFA I in 1992, and subsequent reauthorizations, have addressed these challenges. Specifically, PDUFA authorizes FDA to collect industry user fees to, among other things, hire additional staff, and manage and enhance information technology systems. The user fees collected under PDUFA have enabled the Agency to speed the application review process for new drugs and biological products without compromising FDA’s high standards for new drug safety, efficacy, and quality.
Speeding Americans’ Access to Safe and Effective New Therapies
PDUFA revolutionized the United States’ drug approval process. It reversed the lag in drug approvals that prompted its creation, providing Americans with more timely access to safe and effective medical products.
The PDUFA program began with a general focus on shortening review times, and its scope has expanded beyond the time for review of an application. The five-year reauthorization cycles for PDUFA support continuous program innovation, evaluation, and improvement. The enhancements to the process for the review of human drug applications originally focused on the FDA pre-market review of NDAs and BLAs. Through successive PDUFA reauthorizations, program enhancements have evolved and expanded to include extensive communication and consultation between drug sponsors and FDA throughout the drug development process. These enhanced interactions give us the opportunity to provide more guidance to sponsors, including setting clearer expectations of what data are necessary to properly review and evaluate a drug, improving the potential for first-cycle approval, and getting safe and effective drugs to patients sooner – supporting FDA’s mission. These interactions also enable sponsors to incorporate advances in regulatory science into their development programs, expediting drug development and facilitating timely regulatory decisions.
As discussed in more detail below, PDUFA VI included additional resources for breakthrough therapy review to expedite those products that offer early promise of benefit over existing therapies, initiated pilot programs for complex innovative trial designs and model-informed drug development, and expanded the provisions of the 21st Century Cures Act (CURES) in its focus on activities for patient-focused drug development and use of real-world evidence (RWE) in regulatory decision making. The continued modernization of drug review under PDUFA is supported by FDA’s enhancements in informatics and hiring practices, including the Agency’s implementation of hiring authorities under CURES to bring top talent to the Agency enabling us to consistently meet or exceed PDUFA commitments.
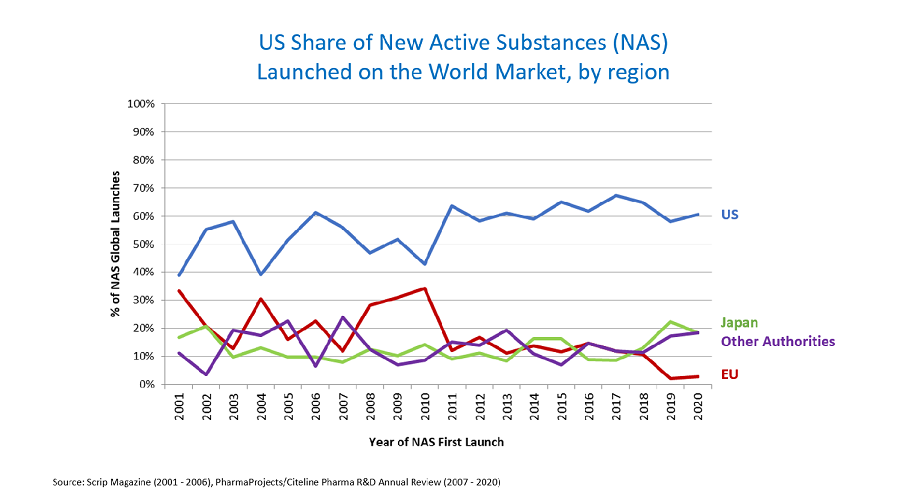
With these enhancements the United States continues to be a global leader in drug innovation and Americans are now typically the first to benefit from new safe and effective medicines. As shown in the figure below, this is a consistent pattern for novel drugs and biological products and while it may also be influenced by other factors, e.g. economics, it would not be possible without a robust approval process that is predictable and efficient.
As shown in Figure 1, today, almost two-thirds of new active substances approved in the world market are launched first in the United States.
FIGURE 1 – U.S. Share of New Active Substance Launched on the World Market, by region
* New active substances (NASs): new chemical or biological entities where the active ingredient had received no prior approval for human use.
Throughout this program evolution, FDA has continued to review large volumes of submissions and to deliver predictably high levels of performance against PDUFA goal commitments for timely regulatory review, as shown in Figure 2, below. This was accomplished even as FDA witnessed an unprecedented increase in submissions during the COVID-19 pandemic, and as FDA facilitated the development of therapeutics and vaccines, resulting in the authorization and approval of numerous COVID-19 vaccines and treatments.
Figure 2 FDA Review Performance - FY 2021: Percent of Submissions Acted on by Goal Date1
*Goal 90%
Increasing the Timeliness and Efficiency of Premarket Review
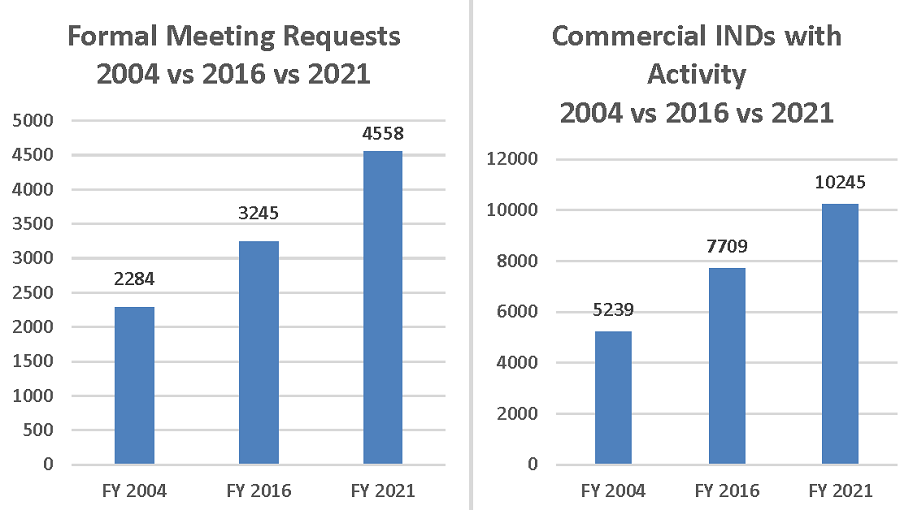
A key element of the success of the PDUFA program is the ongoing development-phase consultation FDA provides to drug sponsors. FDA’s capacity to provide sponsors, including small first-time innovators, with timely advice enabled by PDUFA funding, has contributed to the strong drug development pipeline in the United States today. This is reflected in the increased numbers of drug development programs underway (measured by commercial INDs with activity), and the corresponding growth in company requests for development-phase meetings, as shown in Figure 3.
Figure 3. FY 2004, 2016, and 2021 Formal Meeting Requests and FDA Commercial Investigational New Drug (INDs) with Activity
The volume of formal meetings requested by drug sponsors has steadily grown over the course of PDUFA. Early and frequent communication between sponsors and FDA serves to improve the efficiency of drug development. These meetings help sponsors navigate key milestones during drug development, increase the likelihood of well-designed and executed studies, and enable sponsors to clarify requirements for complete application submissions and potentially avoid the need for an additional review cycle, translating into earlier treatments and cures for patients.
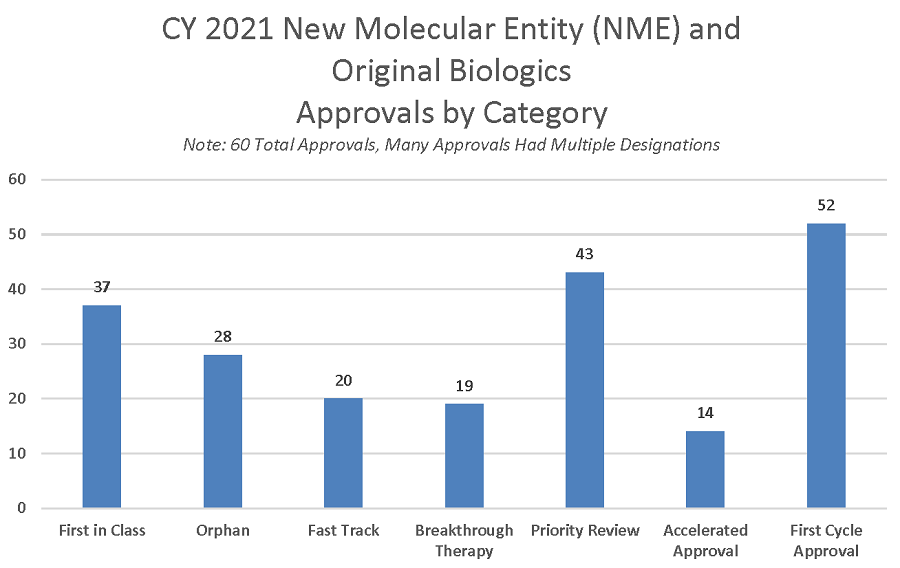
The improvement in the quality of drug development programs and the submitted applications, supported by these PDUFA-enabled consultations, is an important factor that explains the 87 percent first cycle approvals (52 of 60) of applications for new molecular entity (NME) NDAs and BLAs. Figure 4 provides key attributes of NME approvals for the calendar year 2021.
Figure 4: CY 2021 New Molecular Entity (NME) and Original Biologics Approvals by Category
Development-phase consultations can be particularly helpful in support of the most innovative or challenging drug development programs. For instance, of the NME NDAs and original BLAs that FDA approved in calendar year 2021, close to half (47%) were indicated for rare diseases. In addition, over half (61%) of the drugs and biologics approved were first in their class, i.e., drugs and biologics with different mechanism of action from existing therapies.
While the standard review target for NMEs and original biologics submissions that are filed is ten months after the 60-day filing date2, FDA expedites review for eligible drugs through a priority review, with a goal to review drugs within six months after filing. Priority review is generally targeted at drugs for serious conditions that, if approved, would provide significant improvements in safety or effectiveness3. In 2021, 43 of 60 NMEs and original biologics (72%) were designated for priority review.
Many drugs and biological products that receive priority review also benefit from other expedited programs intended to accelerate development, such as fast track designation and breakthrough designation. Both these programs offer greater interactions between sponsors and FDA reviewers throughout the development process, including FDA providing advice on the design and implementation of the clinical trials necessary to demonstrate product safety and effectiveness. In addition, breakthrough designation typically includes greater involvement of FDA leadership. For cell and gene therapies, the Regenerative Medicines Advanced Therapy (RMAT) designation program is designed to expedite the review of cellular and gene therapy, therapeutic tissue engineering product, human cell and tissue product, or any combination product using such therapies for which preliminary clinical evidence indicates that the product has the potential to address unmet medical needs for such disease or condition. RMAT designated products receive the same benefits as breakthrough therapies and approval of cell and gene therapies that have RMAT designation may be able to fulfill post-approval requirements by other than traditional clinical studies.
Accelerated approval, another expedited program, also speeds the development process by shortening premarket clinical trials using a surrogate endpoint reasonably likely to predict clinical benefit with a requirement to confirm clinical benefit in the post market setting. Thirty-nine of the 60 NME approvals of 2021 (65%) used one or more expedited programs, specifically fast track designation, breakthrough designation and/or accelerated approval.
COVID-19
As part of the government-wide response to the COVID-19 pandemic, the Agency has been working around the clock over the past two years to facilitate the development and availability of therapeutics and vaccines as expeditiously as possible. FDA accelerated the development and publication of guidance and other information for industry and researchers on developing COVID-19-related treatments and vaccines.
In March 2020, FDA announced the creation of an emergency review and development program for possible therapies for COVID-19, the Coronavirus Treatment Acceleration Program, or “CTAP.” The primary goal of CTAP is to help accelerate the development of therapeutics for patients and consumers. The Agency supported the program by reassigning staff and working continuously to review requests from companies and researchers who are working to develop therapies. Under CTAP, FDA is using every available authority and appropriate regulatory flexibility to facilitate the development of safe and effective products to treat patients with COVID-19. As of December 31, 2021, there were more than 670 drug development programs in the planning stages and we reviewed more than 470 trials of potential therapies for COVID-19. These include antivirals, immunomodulators, neutralizing antibodies, cellular and gene therapies, and combinations of these products. The diversity of therapeutic approaches being investigated is important because it rapidly expands our understanding of the effect of different categories of potential treatments. In addition, drugs have been identified that meet the standard for emergency use authorization, and FDA has acted to make these products available while continuing to collect information about their safety and effectiveness. As of January 31, 2022, the Agency authorized 14 drugs and non-vaccine biological products and approved one antiviral drug. Notably, these drugs are authorized or approved for the continuum of medical needs, from pre- and post-exposure prophylaxis, to treatment of outpatients with mild-moderate disease, to treatment of hospitalized patients with severe or critical COVID-19.
FDA has authorized three COVID-19 vaccines. All three vaccines are authorized for individuals 18 years of age and above with one of these vaccines authorized for individuals as young as five years of age. One vaccine is also approved for individuals 16 years of age and above and another for individuals 18 years of age and older.
In addition to providing access through authorizations and approvals, since the start of the pandemic, CDER has authorized over 2,100 expanded access requests for COVID-19 therapeutics, including emergency requests and CBER authorized 6,306 expanded access requests, 6,084 (96%) of which were in support of COVID-19 convalescent plasma.
Over the past two years, FDA has continued to work at a pace that is unprecedented, and not sustainable outside of an emergency, to deliver authorized and approved therapeutics and vaccines with unparalleled speed to the meet critical public health needs. Notwithstanding the increased workload, the average time between the request and meeting with sponsors for COVID-19 products was reduced by 50 percent. Although not all COVID-19 work is supported by user fees, without the staff, expertise and infrastructure provided by PDUFA user fees, our COVID-19 efforts would have been impossible to carry out. Furthermore, it is a testament to the seriousness with which we take our commitments under PDUFA that we continued to succeed in meeting key PDUFA commitments in the face of a large increase in non-PDUFA COVID-19 work. For instance, in fiscal year 2020 FDA received 46 percent more new INDs and 26 percent more formal meeting requests compared to fiscal year 2019.
PDUFA VI - Fulfilling Our Commitments
We are currently in the final year of the PDUFA VI program. Since the enactment of PDUFA I in 1992, the complexity of scientific and clinical issues in the study of new drugs has grown, including the use of genetic targeting, biomarkers, novel trial designs, and plans and programs to ensure effective post-market risk management relying on the Sentinel system, one of the largest RWE sources in the United States. In addition, PDUFA has enabled FDA to provide increased communication and consistent guidance during drug development and application review, a top priority for drug sponsors.
PDUFA VI (FY 2018 to FY 2022) built upon the achievements of PDUFA V and committed the Agency to numerous initiatives to ensure the continued success of the human drug review program including:
- Capturing the patient voice in drug development;
- Ensuring sustained success for breakthrough therapies;
- Enhancing biomarker development;
- Advancing the use of complex innovative trial designs and model-informed drug development;
- Streamlining the review of combination products;
- Enhancing the use of RWE;
- Hiring and retaining highly qualified staff; and
- Enhancing the management and transparency of user fee resources.
The Agency’s progress on these priorities is detailed below.
Capturing the Patient Voice in Drug Development
Elevating patient voices in developing new drugs to treat their diseases and conditions was a central part of PDUFA VI. The commitments in PDUFA VI complemented the patient focused-drug development (PFDD) provisions in the CURES Act by leveraging essential patient input and insights to fight disease.
Under the PDUFA VI authorization, the Agency focused on a series of four methodological PFDD guidance documents to address, in a stepwise manner, how stakeholders can collect and submit patient experience data and other relevant information from patients and caregivers. This series of guidance documents is intended to facilitate the advancement and use of systematic approaches to collect and use robust and meaningful patient and caregiver input that can better inform medical product development and regulatory decision making.
In addition, over the course of PDUFA VI, FDA engaged with patient advocacy groups to support their conduct of 54 externally led PFDD meetings and convened five public workshops to allow the patient voice to inform not only the above guidances but other disease specific development programs.
Ensuring Sustained Success for Breakthrough Therapies
The Breakthrough Therapy designation program is designed to expedite the review of therapies for serious conditions that show preliminary clinical evidence of a substantial improvement on a clinically significant endpoint over available therapy. This program has become a critical component of the human drug review program with requests and designations far exceeding expectations. PDUFA VI sought to ensure the sustained success of the breakthrough program by investing additional resources into the program. For the first four years of PDUFA VI, FY 2018 – FY 2021, FDA received 586 breakthrough requests and granted 248. Drugs approved during PDUFA VI with breakthrough therapy designation include many new options for both adult and pediatric patients with cancer. Targeted oncological therapies with breakthrough designation included treatment for metastatic cancers with NTRK fusion proteins and a host of new treatments for non-small cell lung cancer targeting clinically relevant biomarkers – ALK, EGFR, MET, RET and KRAS. In addition, novel treatments with breakthrough designation were approved across many other cancers including breast cancer, bladder cancer, lymphoma, cholangiocarcinoma and rare tumors such as tenosynovial giant cell tumor and plexiform neurofibromas. Rare disease approvals during this period included the first triple therapy for the most common cystic fibrosis mutation, the first therapy to treat heart disease (cardiomyopathy) caused by transthyretin mediated amyloidosis, treatment for Hutchinson-Gilford progeria syndrome, and the first therapy for thyroid eye disease.
Enhancing Biomarker Development
FDA and industry share the goals of the CURES Act and PDUFA VI to accelerate development of reliable biomarkers to advance important new therapies. Biomarkers are currently used throughout the drug development process, including as surrogate endpoints to support earlier evidence of effectiveness for regulatory decision-making when evidence from a clinical endpoint could take much longer or require many more patients to be studied
A surrogate endpoint that is well established to predict clinical benefit, such as blood pressure as a predictor of risk of stroke, or viral load in certain infectious diseases, is considered validated and can be used to support traditional approval. Other surrogate endpoints are those for which there is evidence that they are reasonably likely to predict an improvement in a clinical outcome. Such surrogate endpoints may be used to approve a drug under accelerated approval for a serious or life-threatening disease for which there are not adequate therapies. For accelerated approvals, FDA requires post-marketing studies to verify the expected clinical benefit. FDA publishes a list of surrogate endpoints that have been used to support drug approval or licensure that includes whether the surrogate endpoint was used to support traditional or accelerated approval4.
Meaningful progress in developing additional biomarkers for public qualification requires a sustained effort and collaboration among a wide range of stakeholders. The Agency continues to have success via the Biomarker Qualification Program. In 2018, FDA qualified two additional biomarkers, one a safety biomarker panel to aid in the detection of kidney injury in early trials and the second a biomarker to monitor malaria treatment. Other promising biomarkers have progressed to the Qualification Plan stage, including biomarkers for important diseases such as inflammatory bowel disease, Parkinson’s disease, emphysema, non-alcoholic steatohepatitis, osteoporosis and others. FDA continues to work with the National Institutes of Health, the Biomarkers Consortium, the Critical Path Institute and others to advance biomarker development under PDUFA VI.
Streamlining the Review of Combination Products
More streamlined review of combination products is another FDA and industry priority reflected in PDUFA VI. Combination products are therapeutic and diagnostic products that contain two or more types of medical products as constituent parts: a drug and device, a drug and biologic, a biologic and device, or all three (drug, biologic, and device).
Under PDUFA VI, FDA assessed combination product review practices. Based on the resulting recommendations, FDA pursued improvements in inter-center and intra-center combination product review coordination, consistency, and transparency for PDUFA products that are combination products regulated by CDER and CBER (PDUFA combination products), including through IT enhancements and training. FDA published several guidances regarding combination products to review more efficiently, effectively, and consistently combination products, including guidance that describes the ways in which combination product sponsors can obtain feedback from FDA on scientific and regulatory questions as well as best practices for FDA and sponsors when interacting on these topics.5
Advancing the Use of Complex Innovative Trial Designs and Model-Informed Drug Development
FDA routinely works closely with industry to facilitate innovative approaches to drug development that maintain our high standards for drug safety and efficacy. PDUFA VI encouraged these efforts by advancing Model-Informed Drug Development (MIDD) and the use of Complex Innovative Trial Designs (CID).
To fulfill the goals and commitments of PDUFA VI, the Agency developed the MIDD Pilot Program6 and the CID Pilot Meeting Program7.
The MIDD Pilot Program is designed to:
- Provide an opportunity for drug developers and FDA to discuss the application of MIDD approaches to the development and regulatory evaluation of medical products in development; and
- Provide advice about how particular MIDD approaches can be used in a specific drug development program.
Under the pilot program, FDA accepts two to four paired-meeting requests for meetings each quarter. For each meeting request granted as part of the pilot, FDA conducts an initial and follow up meeting on the same drug development issues to occur within a span of approximately 120 days. Under the pilot program from FY 2018 – FY 2021, FDA received 46 meeting requests and granted 38 of those requests. The total number of sponsor meetings during that time period was 43. The meeting requests spanned 14 different therapeutic areas – cardiology, oncology, non-malignant hematology, neurology, infectious disease, immunology/inflammation, dermatology, pulmonary, psychiatry, gastroenterology, ophthalmology, endocrinology, nephrology, and hepatology.
The CID Pilot Meeting Program developed under PDUFA VI is designed to:
- Facilitate the use of complex adaptive, Bayesian, and other novel designs in late-stage drug development; and
- Promote innovation by allowing FDA to publicly discuss the trial designs considered through the pilot meeting program, including trial designs for medical products that have not yet been approved by FDA.
Under the pilot meeting program, FDA accepts up to two meeting requests per quarter yearly. For each meeting request granted as part of the pilot, FDA conducts two meetings on the proposed CID within a span of approximately 120 days. From FY 2018 – FY 2021, the CID pilot program received 15 meeting requests - 13 for CDER and 2 for CBER - and granted five of the CDER meeting requests. The total number of sponsor CID meetings was 16, as FDA granted additional meetings during the 120-day span. The meeting requests spanned seven different therapeutic areas – neurology, oncology, malignant hematology, non-malignant hematology, pain, rheumatology, and gastroenterology.
Enhancing the Use of Real-World Evidence (RWE)
Medical care and biomedical research are amid a major transformation with data from electronic health records, insurance claims databases, patient registries, digital health technologies, and other new sources comprising an immense new set of information about health and healthcare. Sponsors and the research community are seeking to take advantage of the quantity of data generated in routine medical practice to help inform regulatory decisions about the safety and effectiveness of drugs. Importantly, these real-world data (RWD) sources provide data about patients outside of structured clinical trial visits and in the social context of their day-to-day lives. These sources of data are now becoming increasingly available to researchers, clinicians, and patients with the potential to improve medical care and public health.
FDA recognizes the potential value of utilizing RWD to generate RWE in evaluating not only the safety of medications but also their effectiveness. Under PDUFA VI, the Agency continues to fulfill our commitment to enhance the use of RWE. The Agency has conducted multiple demonstration projects, engaged with external stakeholders, and to date published four guidances on the use of RWE in regulatory decision-making. For example, FDA published draft guidance with recommendations on using data from electronic health records, medical claims, registries, and data standards for applicable submissions containing study data derived from RWD sources. In addition, another draft guidance describes regulatory considerations for the design and conduct of non-interventional (or observational) studies.
Hiring and Retaining Highly Qualified Experts
To efficiently conduct reviews of human drug applications and meet PDUFA commitments, FDA must be able to hire and retain sufficient numbers and types of technical and scientific experts. To strengthen this core capability during PDUFA VI, FDA established a modernized position management system, more efficient recruiting practices, a dedicated scientific recruiting function and metric goals for human drug review staff hiring. We also conducted a comprehensive independent assessment of hiring and retention system performance. The Agency thanks the Committee for providing vital hiring authorities in the CURES Act, greatly improving FDA’s ability to hire and retain scientific experts in more complex and specialized areas and meet our growing responsibilities.
The Agency continues to put every effort into meeting our hiring goals under PDUFA VI. FDA is committed to hiring 230 Full-Time Equivalents (FTEs) from FY 2018 to FY 2022 as agreed upon in the PDUFA VI commitment letter. FDA has successfully hired 212 FTEs of the 230 FTEs (92%) as of September 30, 2021.
Enhancing the Management of User Fee Resources
FDA is committed to enhancing management of PDUFA resources and ensuring PDUFA user fee resources are administered, allocated, and reported in an efficient and transparent manner. Under PDUFA VI, the Agency established a resource capacity planning function to improve its ability to analyze current resource needs and project future resource needs, modernized its time reporting approach (e.g., ~99% of CDER and CBER employees time report), conducted an evaluation of PDUFA program resource management, and published a five-year PDUFA financial plan with annual updates8.
In 2020, FDA embarked on its own initiative – not a PDUFA commitment – to modernize the New Drugs Regulatory Program9. These changes are intended to improve efficiency and consistency of our work to free up resources so that our scientists have more time to focus on the increasing challenges of drug development, particularly for unmet medical needs, and on the multiple collaborations needed to make sure candidate drugs are developed and assessed properly, with appropriate input from external scientists, expert physicians, and patient communities. The initiative includes regulatory and review process changes, as well as organizational restructuring and strengthening the institutional support structures, including personnel and information technology (IT), that underpin the regulatory process.
PDUFA VII Reauthorization
As part of PDUFA VI, Congress directed the Agency to reach out to all stakeholders to solicit thoughts and insights on PDUFA reauthorization and changes to PDUFA performance goals. FDA followed the process, as described in statute, in developing the recommendations for reauthorization. This included holding two public meetings, conducting negotiations with the regulated industry, and having regular consultations with stakeholders, including patient and consumer advocates. To ensure transparency in this work, the Agency posted the meeting minutes for the various engagements, including: the two public meetings; over 100 negotiation sessions with industry, and six stakeholder discussions10.
PDUFA VII Overview
Based on the maturity and success of the PDUFA program, the recommendations for PDUFA VII focus on ensuring FDA has capacity to review new and innovative products, including cell and gene therapy products. To provide the capacity needed to successfully implement the commitments outlined below, while maintaining current performance, PDUFA VII recommends increasing fees to fund 352 new staff and to support critical investments in program infrastructure, such as data IT modernization. The new staff and investments are scheduled to phase in over the five years of PDUFA VII. The commitments thematically fall into the following categories:
- Enhancing CBER’s capacity to support development, review, and approval of cell and gene therapy products and new allergenic extract products;
- Improving pre-market review processes and procedures;
- Enhancing regulatory science to expedite drug development;
- Enhancing regulatory decision tools to support drug development and review;
- Continuing enhancement and modernization of the drug safety system;
- Enhancing product quality reviews, chemistry, manufacturing, and controls (CMC) approaches, and advancing the utilization of innovative manufacturing technologies;
- Continuing enhancements for management of user fee resources;
- Improving FDA’s hiring and retention of key scientific and technical talent; and
- Enhancing IT and bioinformatics goals.
Enhancing CBER’s capacity to support development, review, and approval of cell and gene therapy products and new allergenic extract products
FDA has experienced exponential growth in cellular and gene therapy submissions over the past 7 years with over 1,993 active, development programs. We have seen a sustained increase in development program activities, including an 85 percent increase in original IND receipts, a 139 percent increase in IND amendment receipts, and a 158 percent increase in formal meeting requests. In addition, the RMAT program has advanced the development of a wide variety of cellular and gene therapies with many including orphan designations and for pediatric populations. From program initiation in December 2016 through 2021, 68 of 180 requests have received RMAT designation with three RMAT designated products receiving approval in 2021 - two allogenic cellular products, one for immune reconstitution in pediatric patients with congenital athymia, one for wound healing, and a CAR-T gene therapy for B-cell lymphoma.
Therefore, PDUFA VII proposes new enhancements to CBER’s capacity to support development, review, and approval of cell and gene therapy products to accommodate the current and expected influx of work in the coming years. The proposal will support development of multiple guidances, numerous public meetings to examine new technologies and approaches, patient-focused drug development meeting to better understand patient perspectives on gene therapy products, and public outreach to facilitate product development and approval. In addition, if the negotiated commitments are adopted, new allergenic extract products will be included in PDUFA VII, and the program will provide needed resources to facilitate the development and approval of new therapies, including those for food allergens, which constitute most new allergenic products under development.
Improving pre-market review processes and procedures
Communication during drug development continues to be critical to successful drug development. PDUFA VII proposes several enhancements to the current robust communication framework. PDUFA VII proposes exploring a new pilot program for certain efficacy supplements, i.e., when a sponsor is seeking a new indication for an already approved product that would support review earlier than would otherwise occur with the goal of expediting patient access to novel uses for existing therapies. The proposal also seeks to expand communication and feedback during the drug development process by creating two new formal meeting types and allowing for follow-up opportunities after meetings.
Finally, the commitment letter also includes new performance goals for pre-approval review of postmarketing requirements (PMRs), studies done after a drug is on the market to further explore efficacy and or safety to ensure timely availability of information on the safety and efficacy of therapies. In addition, it includes a new process for reviewing sponsor-initiated requests to release the applicant from the requirement to perform a PMR study.
Enhancing regulatory science and decision tools to expedite development
Model-Informed Drug Development (MIDD) and Complex Innovative Design (CID)
PDUFA VII proposes to further enhance regulatory science and to expedite drug development by continuing FDA’s successful CID and MIDD programs. Specifically, the proposed CID program will continue to facilitate the advancement and use of complex adaptive, Bayesian, and other novel clinical trial designs. The MIDD program will also continue to further advance and integrate the development and application of exposure-based, biological, and statistical models in drug development and regulatory review.
Advancing Development of Drugs for Rare Diseases
In addition, building on the success of the rare disease programs in CDER and CBER, a new pilot program will be launched to advance rare disease drug development by providing a mechanism for sponsor discussion with FDA to facilitate the endpoint development process—often a critical challenge in efficient trial design.
Advancing RWE for Use in Regulatory Decision-Making
FDA will also build on its current RWE program with a new pilot program that seeks to improve the quality and acceptability of RWE-based approaches in support of new labeling claims, including approval of new indications of approved medical products, or to satisfy post-approval study requirements.
Enhancing Use of Digital Health Technologies to Support Drug Development
Recognizing the growth of digital health technology (DHT) and that remote data acquisition from patients and clinical trial participants has the potential to measure a wide range of activities, behaviors, and functioning in real-life settings that can inform important clinical endpoints, PDUFA VII proposes to establish a framework to guide the use of DHT-derived data in regulatory decision making. FDA will undertake workshops and demonstration projects to inform this work and will address standardized processes for data management and analysis of large databases from digital health tools.
Furthering the Patient Voice in Drug Development
PDUFA VII proposes to continue to enhance decisions to support drug development and regulatory review by advancing the patient’s voice in drug development and decision-making through PFDD, including training and public workshops, and issuing guidance on the use and submission of patient preference information.
Furthering the Review of Combination Products
As noted, under PDUFA VI, the Agency took steps to facilitate the review and approval of combination products. PDUFA VII would add to these activities by introducing new procedures and timelines for use-related risk analysis and human factor validation study protocols as part of the combination products review process.
Continuing enhancement and modernization of the drug safety system
PDUFA VII proposes to continue enhancement and modernization of FDA’s robust drug safety system by modernizing and improving Risk Evaluation and Mitigation Strategy assessments, including updates to guidances, policies and procedures, and new review performance goals. The proposal will optimize the Sentinel Initiative capabilities by enhancing analytic functions to help inform labeling on the safety of product use in pregnancy, to detect safety signals in a timely manner, and to advance the understanding of how RWE can be used to study effectiveness.
Enhancing product quality reviews, chemistry, manufacturing, and controls (CMC) approaches, and advancing the utilization of innovative manufacturing technologies
PDUFA VII proposes new enhancements related to product quality reviews, chemistry, manufacturing, and controls (CMC) approaches, and advancing the utilization of innovative manufacturing technologies by enhancing communication to promote more efficient and effective review through more structured CMC information requests. Also included is a commitment to notify sponsors in advance of facility inspections where FDA needs to see the product being manufactured. Under the proposal, the Agency will issue guidance on FDA’s thinking on the use of alternative tools to assess manufacturing facilities included in pending applications (such as alternative tools utilized during the COVID-19 pandemic). The proposal will also initiate a new pilot program to facilitate and expedite CMC development for products with accelerated clinical development timelines. Lastly, PDUFA VII proposes to advance the utilization and implementation of innovative manufacturing technologies through a public workshop and a published strategy document.
Continuing enhancements for management of user fee resources
PDUFA VII proposes to continue to enhance management of user fee resources by advancing FDA’s resource capacity planning function and adjustment methodology, including a third-party evaluation of the methodology by 2025. The proposal will continue financial transparency by FDA issuing a five-year financial plan and annual updates and holding annual public meetings to discuss PDUFA finances.
Improving FDA’s hiring and retention of key scientific and technical talent
PDUFA VII proposes to further improve FDA’s hiring and retention of key scientific and technical talent. FDA commits to report on FDA’s website progress on annual PDUFA VII hiring goals. FDA also commits to utilizing an independent contractor to conduct a targeted assessment of the hiring and retention of staff for the human drug review program and will post this assessment on FDA’s website.
Enhancing IT and bioinformatics goals
PDUFA VII proposes to enhance IT and bioinformatics by enhancing transparency of IT activities and modernization plans through regular meetings, publishing a data and technology modernization strategy, and engaging with external stakeholders on initiatives around data convergence. The proposal will modernize the Electronic Submission Gateway, explore cloud and cloud-based technologies, and leverage modern technology to accelerate CBER’s data and technology modernization. Additional staff and resources are added in PDUFA VII to support review and analysis of the increasing amounts of bioinformatics and computational data submitted during product development and review, including the management of submissions with extensive and continuous data from digital health technologies.
GDUFA
GDUFA has helped to significantly expand the timely availability of and patient access to affordable, high quality generic medicines since its inception. Patient confidence that generic drugs will work the same as brand products, and can be freely substituted, is the foundation for trillions of dollars in savings that generics have produced for the healthcare system.
The generic drug industry has grown from modest beginnings in 1984 into a major force in health care to reduce health care costs. In the past ten years (2011-2021) close to 1,000 first generic medicines have been approved, offering patients access to drugs for which there was no previous generic competition. FDA has also approved thousands of additional versions of generic medicines over this time, contributing to significant price reductions for consumers. According to the Association of Accessible Medicines, based on an analysis by IQVIA, generic drugs saved the U.S. health care system $2.4 trillion from 2011 to 2020.11
This success was enabled by the enactment of GDUFA I as part of the Food and Drug Administration Safety and Innovation Act of 2012 and reauthorization of the program (GDUFA II) as part of the FDA Reauthorization Act of 2017. While substantial progress has been made, there is still more to be done. With more generic drugs on the market there is a corresponding increase in the need for FDA regulatory activity over the lifecycle of these products. Indeed, we see a steady increase in approved abbreviated new drug applications (ANDA) with post-approval actions, including Prior Approval Supplements and Changes Being Effected (CBE) submissions (Figure 5). Most of these submissions involve manufacturing facility and labeling updates. In addition, with the steady approval of new molecular entities and innovative new uses for previously approved drugs, including many new complex products, the GDUFA program faces increased industry requests for regulatory feedback to bring the next generation of generic drugs to the market.
Figure 5 – Receipts of Prior-Approval Supplements and Changes Being Effected Submissions by Fiscal Year
GDUFA II - Fulfilling Our Commitments
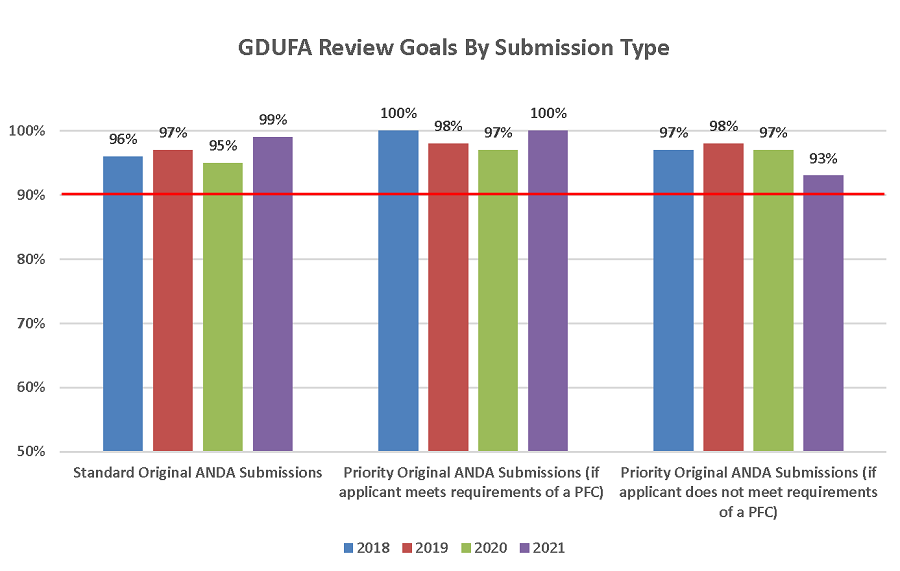
Under GDUFA II, FDA eliminated the backlog of hundreds of ANDAs and made significant progress in timely review of generic drug submissions. In the first four years of GDUFA II we approved over 3000 ANDAs and, to facilitate generic drug development, issued over 50,000 communications to industry. Under GDUFA II, the Agency committed to assess 90 percent of priority ANDAs within eight months of submission and to assess 90 percent of standard ANDAs in ten months. The program has surpassed its 90 percent goal for assessment of all original standard and priority ANDAs (Figure 6) and continued to meet or exceed the majority of its goals even during the COVID-19 pandemic, with over 1300 approvals for drug products used to treat patients suffering from COVID-19. For many of these COVID-19 approvals, the decision was made in less than half the applicable goal period. In addition, throughout GDUFA II, approximately 13 percent of annual ANDA approvals were for complex generics including the first generic inhaler for asthma and chronic obstructive pulmonary disease.
Figure 6 – Achievement of GDUFA II Review Goals by Submission Type
PFC – those applicants who met the requirements of the Pre-Facility Correspondence process (21 U.S. C. 355(j)(11)).
90% goal for all submission types
Faster assessment of priority ANDAs
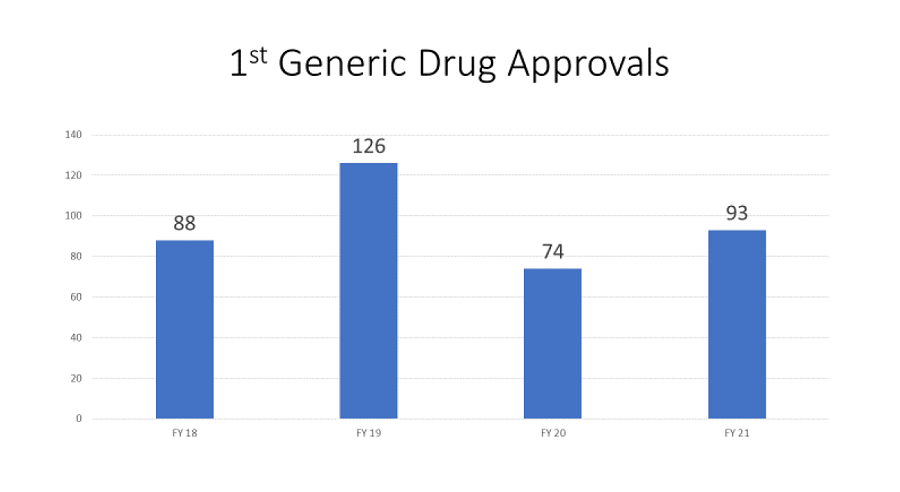
Under amendments made by the FDA Reauthorization Act of 2017 (which authorized GDUFA II), priority review is available for applications for generic drugs with limited competition, as well as for generic drugs in shortage, that meet certain conditions. This includes the shorter review timeframe under the Pre-Facility Correspondence (PFC) framework, under which sponsors submit information about manufacturing facilities and testing of the drug not later than 60 days prior to the submission of the application. In addition, a core element of prioritization efforts under the GDUFA II commitment letter is to expedite the assessment of potential “first generic” ANDAs because they can open the market to generic competition for the first time. Many “first generic” ANDAs cannot lawfully be submitted until a specific date after the innovator drug was approved. Figure 7 shows the number of first generic drug approvals by fiscal year (FY) during GDUFA II.
Figure 7 – First Generic Drug Approvals by Fiscal Year
To provide some clinical context for these numbers, Table 1 provides a summary of some significant first generic approvals for CY 2021.12
Table 1 – Significant First Generic Drug Approvals in CY 2021
| Generic Name | Brand Name | Indication | Approval Date |
| Linaclotide Capsules | Linzess Capsules | Irritable bowel syndrome with constipation and chronic idiopathic constipation | 2/9/2021 |
| Apremilast Tablets | Otezla Tablets | Moderate to severe plaque psoriasis | 2/18/2021 |
| Ibrutinib Capsules | Imbruvica Capsules | Mantle cell lymphoma (MCL) | 3/31/2021 |
| Enzalutamide Capsules | Xtandi Capsules | Prostate cancer | 5/14/2021 |
| Lenalidomide Capsules | Revlimid Capsules | Multiple myeloma, anemia, and certain lymphomas | 5/21/2021 |
| Tofacitinib Tablets | Xeljanz Tablets | Certain types of arthritis and ulcerative colitis | 6/1/2021 |
| Difluprednate Opthalmic | Emulsion Durezol | Inflammation/pain associated with ocular surgery and treatment of endogenous anterior uveitis | 8/9/2021 |
| Varenicline Tablets | Chantix Tablets | Smoking cessation | 8/11/2021 |
| Linagliptin Tablets | Tradjenta Tablets | Type 2 Diabetes Mellitus | 8/31/2021 |
| Lenalidomide Capsules | Revlimid Capsules | Multiple myeloma | 10/14/2021 |
| Dasatinib Tablets | Sprycel Tablets | Chronic myeloid leukemia | 11/23/2021 |
Pre-ANDA Program Enhancements
To reduce the number of cycles to approval, particularly for complex generic products, the GDUFA II commitment letter established a pre-ANDA program. This program helps clarify regulatory expectations for prospective applicants early in product development, assists applicants in the development of more complete submissions, and provides mechanisms for consultation regarding these products after the ANDA is submitted, thus promoting a more efficient and effective development and assessment process.
As detailed in the commitment letter, the GDUFA II pre-ANDA program established three types of meetings for complex products:
- Product development meetings in which FDA provides targeted advice concerning an ongoing ANDA development program.
- Pre-submission meetings, which give applicants an opportunity to discuss and explain the content and format of an ANDA before it is submitted.
- Mid-review-cycle meetings, which occur, as the name implies, around mid-cycle after the applicant has received FDA’s assessment of any deficiencies in the application and provides the applicant an opportunity to discuss those concerns and plan for next steps.
During GDUFA II, the Agency has continued to grant these meetings and provided industry further information via the final guidance titled “Formal Meetings Between FDA and ANDA Applicants of Complex Products Under GDUFA Guidance for Industry,” released in November 2020.13
To facilitate development of new generic products, FDA issued Product Specific Guidances (PSGs) to assist the generic pharmaceutical industry with identifying the most appropriate methodology for generating the evidence needed to support ANDA approval, for both complex and non-complex drugs. Under the GDUFA II commitment letter, FDA established goals for issuing PSGs for non-complex new molecular entities. FDA has consistently met this goal and as of January 15, 2022, there were currently 1,949 PSGs available to industry.14
While the GDUFA II commitment letter did not include a goal around PSGs for complex generics, GDUFA supports a robust regulatory science program that supports the development of additional innovative methodologies and more efficient tools to help establish drug equivalence standards and support the development of, and access to, new generic drug products. FDA consults with and solicits input from the public, industry, and academic researchers to develop an annual list of the GDUFA regulatory science initiatives specific to research on generic drugs. In addition, we engage stakeholders through numerous scientific workshops and publish an annual report on accomplishments.15
Another tool in the pre-ANDA program is controlled correspondence, which allows potential applicants to submit targeted questions regarding their drug development program and receive a response within a specific timeframe. Under the GDUFA II commitment letter, FDA made enhancements to its Inactive Ingredient Database, which is an important tool for generic drug developers, to enable users to perform electronic queries to obtain Maximum Daily Intake and Maximum Daily Exposure information for each route of administration for which data are available.
ANDA Assessment Program Enhancements
Consistent with the statute, the GDUFA II commitment letter refined programmatic timeframes, including for sponsor communications, used in the ANDA assessment process. The ANDA assessment program starts with submission of an ANDA. When an ANDA is submitted, FDA first determines whether an ANDA is sufficiently complete to permit a substantive assessment. These “receipt” determinations are made within consistent timeframes. The Agency also increased receipt-related communications to facilitate the receipt decision and resolve certain receipt disputes within consistent timelines.
When a new ANDA is received and is under assessment, FDA communicates assessment deficiencies beginning at approximately the mid-point of the review. Communications continue on a rolling basis during the assessment. When deficiencies in an ANDA prevent FDA from approving it, FDA issues a Complete Response Letter (CRL) itemizing the deficiencies that must be corrected for the ANDA to be approved. The GDUFA II commitment letter established post-CRL teleconferences to allow applicants to seek clarification concerning deficiencies identified in CRLs. This helps applicants meet FDA’s expectations when an ANDA is re-submitted for additional review. In 2021, FDA conducted 73 such teleconferences, 98 percent within 30 days of receipt of the written request.
Drug Master File (DMF) Assessment Program Enhancements
Type II DMFs are submissions from a third party other than the ANDA applicant that contain confidential information on a drug substance (or active pharmaceutical ingredient (API)) or drug substance intermediate (or materials used in their preparation) that the Agency evaluates independently. These submissions can be cross referenced by multiple applicants to support approval of their respective ANDAs. Effective communication between ANDA applicants, DMF holders, and FDA is essential to reduce the likelihood of potential problems that could delay approvals. The GDUFA II commitment letter featured new and enhanced mechanisms to facilitate this communication, including first adequate letters to indicate a DMF has no open issues related to the assessment of a referencing ANDA, no further comment letters, and expanded opportunities for DMF holders to request teleconferences with FDA regarding first cycle DMF deficiency letters.
Pursuant to the GDUFA II commitment letter, FDA issued a draft guidance16 on post-approval changes to a Type II API DMF and submission mechanisms for ANDA applications which reference a Type II API DMF. FDA also issued a revised draft guidance titled “Completeness Assessments for Type II API DMFs under GDUFA.”17
Facility Assessment Enhancements
To mitigate export-related challenges identified by U.S.-based API manufacturers, the GDUFA II commitment letter called for FDA to issue guidance and conduct outreach to foreign regulators on its risk-based manufacturing site selection model. To fulfill this commitment, we issued a manual of policy and procedures (MAPP) titled, “Understanding CDER’s Risk-Based Site Selection Model”18 in 2018, to explain how FDA determines which manufacturing facilities to prioritize for routine surveillance inspections. To mitigate ANDA sponsor concerns, FDA enhanced the speed and transparency of communications concerning facility inspection outcomes. Specifically, we implemented a process to notify facilities of final facility inspection classifications (i.e., No Action Indicated, Voluntary Action Indicated, or Official Action Indicated) within 90 days from the close of the inspection. In addition to enhanced transparency concerning the compliance status of GDUFA facilities and sites, FDA updates its publicly available facility inspection classification database every 30 days to reflect the most recent surveillance inspection outcomes.19
Accountability and Reporting Enhancements
Under GDUFA II, enhanced information infrastructure and analytics increased transparency and accountability for meeting performance goals and strengthened program management and resource use. FDA developed internal processes to enable improved productivity and performance through regular assessment of progress towards GDUFA II goals. The Agency also enhanced the transparent and efficient administration, allocation, and reporting of user fee resources. We expanded GDUFA program reporting and provide the information on our website “Enhanced Accountability & Reporting.”20 Robust performance reporting enables Congress, industry, and other stakeholders to gauge the generic drug program’s performance on an ongoing basis. FDA also issued a Five-Year Financial Plan in FY 2018 with annual updates21 and held an annual meeting22 on financial transparency and efficiency of the user fee programs. In addition, an independent third party evaluated FDA’s Capacity Planning Adjustment (CPA) methodology that in PDUFA and BsUFA adjusts target revenue annually as needed within a user fee cycle to account for forecasted, sustained increases in workload. This report specifically evaluated whether a proposed CPA methodology could be applied to the GDUFA program and whether corresponding outputs could be applied to the GDUFA program to meet the monitoring and reporting of resource needs of the program.23 As discussed below, industry and FDA agreed to implement a CPA in GDUFA III.
GDUFA III Reauthorization
The accomplishments under GDUFA II continued to foster a strong generic drug market for the American public. For example, there are generic versions of the ten most prescribed medications by total prescriptions in 2020. Despite this success, the average first-cycle approval rate remains around 15 percent. While progress is improving in the approvals of complex generics, about 30 percent of active reference products, that do not have generic competition, are complex products. Therefore, the GDUFA III negotiations focused on building on the successes of GDUFA II by proposing new processes and procedures to achieve earlier cycle approvals and enhancing the pre-ANDA program.
GDUFA III Overview
ANDA Assessments
The GDUFA III commitment letter proposes minimizing issuance of complete response letters (CRL) which, as described above, are letters from FDA to an applicant detailing the deficiencies in an application that must be resolved prior to approval, by:
- Utilizing “Imminent Actions” whenever possible to approve an application within 60 days after the goal date if there is a small issue to resolve or a pending expiration of a reference listed drug patent or exclusivity within that time period;
- Extending goal dates when there is a minor issue that can be resolved within three months of the original goal dates, e.g., addressing a labeling issue; this includes changes in labeling review processes to provide more resources to address late-cycle labeling changes;
- Providing the opportunity to extend the goal date by 6-10 months, depending upon the type of ANDA and need for a pre-approval inspection, if an applicant can respond to a major deficiency before the original goal date; such extensions could shorten the overall time to approval.
The commitment letter also seeks to refine the Pre-Facility Correspondence process for priority ANDAs to focus on the information that is available from applicants’ pre-ANDA submissions to inform FDA’s decision regarding the need for a preapproval inspection, to expand opportunities for applicants to use this process.
Another commitment is to increase opportunities for timely regulatory feedback through the expanded use of controlled correspondence to include, for example, questions related to generic drug development after receipt of a CRL, in addition to the opportunity for a post-CRL teleconference.
Drug Master Files and Manufacturing Facilities
For drug master files the commitment letter proposes expanding opportunities for early assessment of DMFs before certain priority ANDAs are submitted and between review cycles to increase the likelihood that the DMF will be adequate at the same time as the associated ANDA and thereby promote earlier cycle approvals. In addition, there will be new goal dates for FDA’s response time for manufacturing questions submitted by a sponsor using controlled correspondence after their ANDA is approved.
While most facilities are compliant with Current Good Manufacturing Practice requirements, a small number of ANDA manufacturing facilities are not able to gain approval to produce ANDAs for the U.S. market due to significant violations identified during an inspection. To assist manufacturers in resolving such violations more expeditiously, under the GDUFA III commitment letter, eligible generic drug facilities could request a Post-Warning Letter Meeting to obtain preliminary feedback from FDA on the adequacy and completeness of their corrective action plans. Once a facility has completed appropriate remediation action and FDA agrees that the next step is a facility reinspection, there would be a goal around the timing for such reinspection.
Pre-ANDA Program and Regulatory Science
The GDUFA III commitment letter proposes to continue to enhance regulatory science and expedite complex generic drug development by providing additional enhancements to the programs. In addition to the GDUFA II goals around PSGs for new molecular entities, the GDUFA III commitment letter would establish goals around PSGs for NDAs for complex drug products approved during GDUFA III. FDA would also commit to improving transparency regarding the timing for upcoming new and revised PSGs, including the prioritization of PSG development. The commitment proposes allowing qualified ANDA applicants or potential applicants to request a PSG teleconference or meeting to obtain Agency feedback on the potential impact of a revised PSG recommendation(s) on ongoing in-vivo bioequivalence studies.
The meeting types provided under GDUFA II are being enhanced and expanded. The GDUFA III commitment letter proposes providing qualified ANDA applicants with the new option for an Enhanced Mid-Cycle Review Meeting to receive scientific advice with the goal of resolving a more significant scientific deficiency in a single review cycle, with appropriate goal date extensions. The proposal also includes providing qualified ANDA applicants a post-CRL Scientific Meeting in which the Agency may provide scientific advice on possible alternative approaches to address deficiencies related to establishing equivalence identified in a CRL.
Finally, the commitment letter proposes setting goal dates for suitability petitions, under which generic drug applicants can submit ANDAs for drug products that differ from an approved brand drug in new dosage form, strength, route of administration, or active ingredient for products with a combination of more than one active ingredient. These petitions usually are submitted in response to market demand that is not met by an approved brand product. These goal dates would be established starting in FY 2024.
Hiring
To provide the capacity needed to successfully implement the new commitments, while maintaining current performance, the GDUFA III proposal recommends increasing fees to fund 128 new FTEs (to be hired in FY 2023). Under GDUFA III, the Agency will provide transparency with respect to hiring in its five-year financial plan reports.
Enhancement of Management of User Fee Resources
- GDUFA III proposes to enhance the operational agility of the GDUFA program and management of user fee resources through further maturation of the Resource Capacity Planning (RCP) capability and a legislative proposal to establish and implement a Capacity Planning Adjustment (CPA) to be used in annual fee-setting annually starting in FY 2024. The CPA would generally allow for up to a three percent increase in inflation-adjusted target revenue for the fiscal year if there are forecasted, sustained increases in workload. This legislative proposal would also eliminate the statutory final year adjustment and replace it with authority for an operating reserve adjustment, to provide the Agency with the option of increasing revenues to help ensure adequate resources in the case of significant under collection of fees or other disruptions in funding. This operating reserve adjustment would allow the Agency the option to increase fees to maintain an operating reserve of 8-10 weeks' worth of carryover user fees. If projected operating reserves exceed 12 weeks of operating costs, FDA would be required to reduce fees for that fiscal year to reduce the operating reserve to no more than 12 weeks of carryover fees. FDA would provide the rationale for the CPA and operating reserve adjustments in the annual Federal Register notice publishing fee rates for that fiscal year. GDUFA III would continue financial transparency by publishing a five-year financial plan and holding a public meeting to discuss the plan and other financial commitments every fiscal year.
BsUFA
Over the past decade, new biological products have led to significant clinical improvements for patients who have serious and life-threatening medical conditions including cancer, rheumatoid arthritis, and diabetes. It is important for the public health of the U.S. population to have access to safe, effective, and affordable biological products. Biosimilars provide more options for patients, and competition has the potential to lower treatment costs, enabling greater access for more patients. FDA is fully engaged with the development and approval of biosimilar and interchangeable biosimilar products and is applying a scientifically rigorous review process to ensure these products meet approval standards, in conjunction with outreach to prescribers and patients. Healthcare providers and patients consistently emphasize that FDA’s approval of biosimilars should provide assurance that they provide the same treatment benefits as the originator, or reference product. FDA is committed to providing this assurance and recognizes its importance to the future success of the biosimilars program.
Biologics Price Competition and Innovation Act of 2009 (BPCI Act)
Biological products are generally made from living organisms and usually consist of large, complex molecules that cannot be easily copied, in contrast to “small molecule” drugs that are produced through chemical processes and are easier to copy as “generic” drugs. The BPCI Act established an abbreviated approval pathway for biological products shown to be “biosimilar to” or “interchangeable with” an FDA-licensed biological reference product. A biosimilar product is one that is highly similar to the reference product notwithstanding minor differences in clinically inactive components, with no clinically meaningful differences in terms of safety, purity, and potency. An interchangeable product is a biosimilar product that meets the additional requirement of demonstrating that the product is expected to produce the same clinical result as the reference product in any given patient and, for a biological product that is administered more than once to a patient, the risk in terms of safety or diminished efficacy of alternating or switching between the biosimilar and reference product is not greater than the risk of using the reference product without such alternation or switch.
The abbreviated approval pathway permits a biosimilar application to rely, in part, on FDA’s previous determination that the reference product is safe and effective, saving the applicant time and resources and thereby encouraging competition and potentially lowering healthcare costs.
FDA Biosimilar Approvals – Progress Continues
FDA approved the United States' first biosimilar product, Zarxio, on March 6, 2015, two years prior to the most recent reauthorization of the Biosimilar User Fee Act (BsUFA II) under the FDA Reauthorization Act of 2017 (FDARA). When BsUFA II was enacted, there were only five biosimilar products approved for four reference products. During BsUFA II the number has grown to 33 biosimilars for 11 reference products, including two interchangeable biosimilars as of January 19, 2022.24
A recent analysis by IQVIA provides data on potential savings with biosimilars.
For example, the cost of insulin products is a barrier to patients obtaining sufficient supply of this essential drug. Interchangeable biosimilars, like generic drugs, may be substituted for the reference product without the involvement of the prescriber, depending on state pharmacy laws. Pharmacy level substitution may further reduce costs, helping to increase patient access. On July 28, 2021, FDA approved the first interchangeable biosimilar insulin product, indicated to improve glycemic control in adults and pediatric patients with type 1 diabetes mellitus and in adults with type 2 diabetes mellitus. Semglee (insulin glargine-yfgn) is both biosimilar to, and interchangeable with (may be substituted for), its reference product Lantus (insulin glargine), a long-acting insulin analog. On December 17, 2021, FDA approved a second biosimilar to Lantus: Rezvoglar (insulin glargine-aglr). These two biosimilar products move the needle forward in our common goal to help ensure increased access to a critical therapy in the treatment of diabetes for Americans who depend on insulin.
Biological products for the treatment of inflammatory conditions greatly improve patients’ lives. However, treatment can be costly—for example, in 2021, the cost of a year’s supply of Humira was approximately $77,000; equating to about $3,000 per syringe.25 Currently, the seven approved biosimilar products to Humira are not on the market, but some could enter the market in 2023.26 One of these biosimilars was approved as an interchangeable biosimilar product. On October 15, 2021, Cyltezo (adalimumab-adbm), originally approved as a biosimilar in August 2017, was approved as interchangeable with its reference product Humira (adalimumab) for Cyltezo’s approved uses. Cyltezo is the first interchangeable monoclonal antibody.
BsUFA II – Fulfilling Our Commitments
We are currently in the final year of the BsUFA II program. BsUFA has enabled FDA to implement a new review model and expand staff capacity to provide increased communication with companies facilitating biosimilar product development. BsUFA II built upon the successes of BsUFA I and established an application review model like “the Program” established under PDUFA V for new molecular entity new drug applications and original biologics license applications. This new model is intended to promote the efficiency and effectiveness of the first cycle review process and minimize the number of review cycles necessary for approval. The main parameters of the Program include the following: 1) pre-submission meetings, 2) original application submissions, 3) Day 74 Letter, 4) review performance goals (10-month user fee clock starts at 60-day filing date), 5) mid-cycle communications, 6) late-cycle and advisory committee meetings, and 7) assessment of the Program. These changes contributed to the increase in approvals during the first cycle, reaching almost 70 percent during BsUFA II compared to 39 percent during BsUFA I.
Meetings and Collaboration
FDA made modifications to meeting processes and procedures as part of BsUFA II. We published a draft guidance “Formal Meetings Between the FDA and Sponsors or Applicants of BsUFA Products”27 and issued a final guidance on “Best Practices for Communication Between IND Sponsors and FDA During Drug Development”.28 As of January 3, 2022, there are close to 100 active biosimilar development programs and we received meeting requests to discuss the development of biosimilars for 47 different reference products. Because these communications are often opportunities to share information and provide critical advice (e.g., trial design, analytical similarity assessment, nonclinical studies, manufacturing, and facility issues), it is important that interactions be conducted efficiently and consistently, with clear, concise, and timely communication. Issuance of guidance on these topics is intended to further those goals and help to foster an environment where sponsors and FDA can work collaboratively during the biosimilar drug development process.
Strengthening Staff Capacity
The ability to hire and retain qualified staff is critical to facilitating the availability of new safe and effective biosimilars. The BsUFA II commitments supported this priority by strengthening FDA’s staff capacity; modernizing the hiring system infrastructure; improving human resources capacity through use of a dedicated expert contractor; establishing a dedicated function for the recruitment and retention of scientific staff; and setting clear goals for hiring. In addition, FDA committed to conducting a comprehensive and continuous assessment of hiring and retention practices. This increase in staff capacity during BsUFA II facilitated the development of new regulations and guidance to clarify the biosimilar pathway and to support reviewer training and timely communication with sponsors. This included issuing guidances that are foundational to the biosimilar pathway. FDA has issued draft or final guidance for all guidances listed in the BsUFA II commitment letter.
Lastly, BsUFA II included goals related to the publication of information about biological products. Addressing these goals and commitments, in 2020, FDA released “The Purple Book: Database of Licensed Biological Products,”29 which is a searchable, online database that contains information about FDA-licensed (approved) biological products, including biosimilar and interchangeable products and their reference products. The database provides users with a public-facing database that includes important information about biological products, including information about product presentations, strength, and dosage forms, in addition to other searchable and sortable data fields.
Independent User Fee Structure
Under BSUFA II, FDA successfully implemented an independent user fee structure based on BsUFA I program costs, along with other financial enhancements to improve FDA’s ability to manage program resources and engage in effective long-term planning. FDA also implemented commitments to improve financial transparency and efficiency, including conducting an independent evaluation of BsUFA program resource management30 and issuing a BsUFA five-year financial plan with annual updates31, in addition to the annual financial reports32, and annual public meetings to discuss program finances33.
BSUFA Reauthorization
The statute directs FDA to develop recommendations for BsUFA III for fiscal years 2023 through 2027. To develop these recommendations, FDA consulted with industry and public stakeholders, including scientific and academic experts, health care professionals, and patient and consumer advocates, as directed by Congress. In addition to meetings with industry organizations, FDA held two public meetings on November 19, 2020, and November 2, 2021, to obtain input from public stakeholders. To ensure transparency in this work the Agency has posted the meeting minutes, including the two public meetings and the 13 negotiation sessions with industry. The recommendations for BsUFA III were transmitted to Congress on January 12, 2022.
BsUFA III Overview
Based on successes of the BsUFA program, the BsUFA III commitment letter focuses on many of the top priorities identified by public stakeholders, regulated industry and FDA. The commitments build on the experience gained through the first and second iterations of BsUFA by expanding on existing successful enhancements, refining elements from the existing program, and including new enhancements. Highlights of the proposed commitments are summarized as follows.
Enhancing pre-market review processes, procedures, and performance
BsUFA III proposes to retain the majority of existing review performance goals FDA and industry agree are working well in the program. With 33 approved biosimilar products to date and more anticipated, FDA and industry expect companies will submit more supplements to FDA during BsUFA III for these products and others that may be approved during BsUFA III. As such, BsUFA III proposes new supplement categories, review timelines and performance goals to expedite the review of certain supplements, including the review of safety labeling updates. In addition, this proposal seeks to improve communication and feedback during the development process by modifying two formal meeting types, introducing a new meeting type to focus on a narrower set of issues than other formal meetings to enable faster responses to industry, and introduces a new follow-up opportunity for sponsors to submit clarifying questions after meetings or “Written Response Only” correspondence to ensure sponsor’s understanding of FDA feedback.
Enhancing biosimilar and interchangeable product development and regulatory science
BsUFA III proposes to continue the framework established in BsUFA II by incorporating best practices in FDA-sponsor communication through updates to relevant guidances, Manual of Policies and Procedures (MAPPs), and Standard Operating Policy and Procedures (SOPPs).
BsUFA III includes commitments for the Agency to:
- Issue guidance on FDA’s thinking on the use of alternative tools to assess manufacturing facilities named in pending applications (incorporating best practices, including those in existing published documents, from the use of such tools during the COVID-19 pandemic);
- Notify sponsors in advance of facility inspections where FDA needs to see the product being manufactured; and
- Advance the development of review processes for biosimilar biological-device combination products by introducing new procedures and timelines for use-related risk analysis and human factor validation study protocols.
To further advance the development of safe and effective interchangeable biosimilar products, BsUFA III proposes a focused effort that includes issuing four foundational guidances for the development of interchangeable products; stakeholder engagement through a scientific workshop; and leveraging the new BsUFA III regulatory science program to advance product development, assist regulatory decision-making, and support guidance development for interchangeable biosimilar products.
As proposed, the BsUFA III regulatory science pilot program would be broadly applicable to biosimilar and interchangeable product development. The pilot program would focus on two demonstration projects: (1) advancing the development of interchangeable products, and (2) improving the efficiency of biosimilar product development.
Continuing enhancements for management of user fee resources
Similar to PDUFA VII, BsUFA III proposes to continue to enhance management of user fee resources by advancing FDA’s resource capacity planning function and adjustment methodology, including a third-party evaluation of the methodology by 2025. The proposal would continue financial transparency through issuance of a five-year financial plan with annual updates and holding annual public meetings to discuss BsUFA finances.
Improving FDA’s hiring and retention of key scientific and technical talent
To accomplish the goals set out in the proposed commitment letter, the Agency would hire 15 new employees for FY 2023 and FY 2024. Like PDUFA VII, BsUFA III proposes to further improve FDA’s hiring and retention of key scientific and technical talent by providing transparency on hiring progress by reporting on progress toward meeting annual BsUFA III hiring goals on FDA’s website and conducting a third-party assessment of FDA’s hiring and retention.
Enhancing IT goals
Similar to PDUFA VII, BsUFA III proposes to enhance transparency of IT activities and modernization plans, including by publishing a data and technology modernization strategy. The proposal would also modernize the Electronic Submission Gateway.
Conclusion
User fees are critical to ensuring that FDA has the resources needed to conduct reviews in a timely fashion without compromising the Agency’s high standards – all part of getting safe and effective medical products to patients sooner. The user fee programs are an example of what FDA, Congress, industry, and other stakeholders can achieve when working together towards the same goal. While we have made demonstrable progress in bringing drug and biological products to market as quickly as possible, we know that more work remains to continue to enhance our review processes, including investing in the hiring and retention of scientific talent (particularly in areas of rapid growth such as cell and gene therapy), maximizing the use of new tools and regulatory science, and investing in a bioinformatics infrastructure to support the evolving needs of the programs. The reauthorization of PDUFA, GDUFA and BsUFA will allow FDA to build upon the programs’ demonstrated success, further benefitting patients and affirming our nation’s standing as a global leader in biomedical innovation.
- 1NME = New Molecular Entity; NDA = New Drug Application; BLA = Biologic Licensing Application
- 2There is a 60-day filing review period, which begins on the date FDA receives the application, to ensure the application is substantially complete and meets filing requirements. For non-NMEs the standard review target is 10 months after receipt date not the 60-day filing date.
- 3Priority review is also available for a drug designated as a qualified infectious disease product, certain supplements that propose a labeling change pursuant to a report on a pediatric study, or an application or supplement submitted with a priority review voucher.
- 4https://www.fda.gov/drugs/development-resources/table-surrogate-endpoints-were-basis-drug-approval-or-licensure
- 5https://www.fda.gov/combination-products/guidance-regulatory-information/combination-products-guidancedocuments
- 6https://www.fda.gov/drugs/development-resources/model-informed-drug-development-pilot-program
- 7https://www.fda.gov/drugs/development-resources/complex-innovative-trial-design-pilot-meeting-program
- 8https://www.fda.gov/about-fda/user-fee-reports/user-fee-five-year-financial-plans
- 9https://www.fda.gov/drugs/regulatory-science-research-and-education/reorganization-office-new-drugscorresponding- changes-office-translational-sciences-and-office
- 10https://www.fda.gov/industry/prescription-drug-user-fee-amendments/pdufa-vii-fiscal-years-2023-2027
- 11Analysis done by IQVIA for 1255 generic molecules based on sales data and pre-patent expiry prices of brand name drugs https://accessiblemeds.org/sites/default/files/2021-10/AAM-2021-US-Generic-Biosimilar-Medicines-Savings- Report-web.pdf
- 12Information on approval of first generics is posted on FDA’s first generic drug approvals website: https://www.fda.gov/drugs/drug-and-biologic-approval-and-ind-activity-reports/first-generic-drug-approvals
- 13https://www.fda.gov/media/107626/download
- 14https://www.accessdata.fda.gov/scripts/cder/psg/index.cfm
- 15https://www.fda.gov/drugs/generic-drugs/science-research
- 16https://www.fda.gov/media/84217/download
- 17https://www.fda.gov/regulatory-information/search-fda-guidance-documents/completeness-assessments-type-ii-apidmfs- under-gdufa-guidance-industry
- 18https://www.fda.gov/media/116004/download
- 19https://www.fda.gov/inspections-compliance-enforcement-and-criminal-investigations/inspection-classificationdatabase
- 20https://www.fda.gov/industry/generic-drug-user-fee-amendments/enhanced-accountability-reporting
- 21https://www.fda.gov/about-fda/user-fee-reports/user-fee-five-year-financial-plans
- 22https://www.fda.gov/drugs/news-events-human-drugs/financial-transparency-and-efficiency-prescription-drug-userfee- act-biosimilar-user-fee-act-and
- 23https://fda.report/media/140656/Independent+Evaluation+of+the+GDUFA+Resource+Capacity+Planning+Adjustme nt+Methodology_0.pdf
- 24https://www.fda.gov/drugs/biosimilars/biosimilar-product-information
- 25House Committee on Oversight and Reform – AbbVie report: https://oversight.house.gov/sites/democrats.oversight.house.gov/files/Committee%20on%20Oversight%20and%20Ref orm%20-%20AbbVie%20Staff%20Report.pdf
- 26AbbVie & Allergan, 2020 Annual Report on Form 10-K: https://investors.abbvie.com/static-files/47512e94-a9a4- 4035-8dbc-6eb59116bb05
- 27https://www.fda.gov/regulatory-information/search-fda-guidance-documents/formal-meetings-between-fda-andsponsors- or-applicants-bsufa-products-guidance-industry
- 28https://www.fda.gov/regulatory-information/search-fda-guidance-documents/best-practices-communicationbetween- ind-sponsors-and-fda-during-drug-development
- 29https://purplebooksearch.fda.gov/
- 30https://www.fda.gov/drugs/development-resources/fiscal-year-2018-financial-management-evaluation-human-druguser- fees-assessment-report
- 31https://www.fda.gov/about-fda/user-fee-reports/user-fee-five-year-financial-plans
- 32https://www.fda.gov/about-fda/user-fee-financial-reports/bsufa-financial-reports
- 33https://www.fda.gov/drugs/news-events-human-drugs/financial-transparency-and-efficiency-prescription-drug-userfee- act-biosimilar-user-fee-act-and