Medical Device & Radiological Health Regulations Come of Age
FDA Consumer magazine
The Centennial Edition / January-February 2006
By Carol Rados
Each day when people put in their contact lenses, test their blood sugar levels, turn on their TVs, cook their meals, or punch a button on their cell phones, they are using products regulated by the Food and Drug Administration's Center for Devices and Radiological Health (CDRH). The CDRH protects Americans with safeguards that enable them to go about their daily lives knowing that these medical devices and radiological products are reasonably safe to use and that they work as intended.
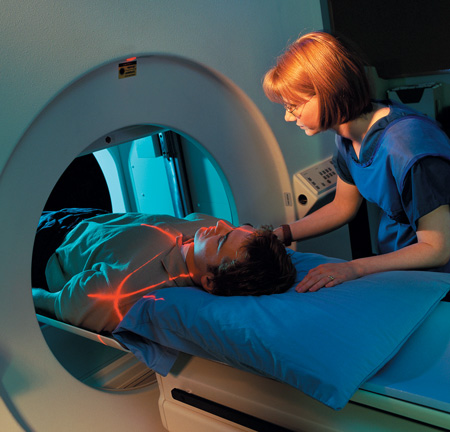
Getty Images
Medical devices are classified and regulated according to their complexity and degree of risk to the public.
By way of distinction, some radiation-emitting products, such as X-ray machines and computed tomography (CT) scanners, are medical devices because they are used in medical procedures. Other radiation-emitting products, such as TVs and microwave ovens, are not used medically, and therefore, are regulated by the FDA under a different law.
Medical devices are classified and regulated according to their complexity and degree of risk to the public. For example, devices that are life-supporting, life-sustaining, or implanted, such as pacemakers, must receive FDA approval before they can be marketed.
But medical devices haven't always come under such scrutiny. In fact, it wasn't until the late 1970s that the FDA actually gained authority to pre- approve medical devices under the 1976 Medical Device Amendments. This law joined a separate law already in existence, the Radiation Control for Health and Safety Act of 1968, which authorized the agency to reduce unnecessary radiation from medical and non-medical electronic products.
Additional laws have, over time, mandated the reporting of adverse reactions to medical devices, post-market monitoring of implants and other devices that pose a serious health risk, recall of dangerous medical devices, and certification and annual inspection of mammography facilities.
The long legal journey toward medical device regulation and radiological health protection--and ultimately the 1976 Medical Device Amendments--begins with the Pure Food and Drugs Act of 1906.
The 1906 act marked the start of federal food and drug legislation designed to protect Americans against threats from harmful substances and deceptive practices. While medical devices were not put into the act, no one could have imagined the ways in which medical device technology would grow, change and, like food and drugs, need to be regulated during the coming years.
A Flood of Fraudulent Contraptions
The earliest recorded fraudulent medical device marketed in the United States was Dr. Elisha Perkins' patent tractors in the late 1700s. Perkins developed two rods of brass and iron about three inches long and sold them throughout the country, claiming they eliminated disease from the body. Even our nation's first president, George Washington, is reported to have purchased a set for his family. Within 10 years of Perkins' death in 1799, the device was exposed as a fraud.
Despite such occasional deceptive enterprises, President Theodore Roosevelt saw no need to ask for legislation concerning medical devices 200 years later, when the Pure Food and Drugs Act was enacted. Devices used by the doctors of his day, such as stethoscopes and scalpels, were comparatively simple, and any hazards or defects were readily apparent. Such devices stood at the edge of medicine--helpful but not essential--and therefore posed little real or perceived threat.
But by 1917, fraudulent medical devices, such as nose straighteners, height-stretching machines, and heated rubber applicators advertised as a cure for prostate gland disorders, began flooding the market. It was clear to the FDA that the law should be expanded to include agency authority over medical devices. In its annual report to Congress that year, the FDA stated that the 1906 act "has its serious limitations … which render it difficult to control … fraudulent mechanical devices used for therapeutic purposes."
Radiation added to the problem. The health hazards of radiation became known soon after the discovery of radium by the French chemists Pierre and Marie Curie in 1898. Before World War I, the FDA was taking action against quack drugs and devices claiming to be radioactive--some of them highly dangerous. Exaggerated health claims, brought to the attention of Congress in a 1926 report, continued for products containing radium. One such device was known as a radium belt, which carried a disc alleged to contain the element. According to proponents, someone wearing the belt would never have appendicitis or gallbladder disease, or perhaps, any other ailment.
Most of the FDA enforcement activity at the time was concerned with getting fraudulent devices like these off the market. While the agency continued to monitor the products and assist the Federal Trade Commission and the U.S. Post Office--both charged with overseeing devices and enforcing criminal penalties for mail fraud under the Postal Fraud Statutes--the FDA could take no action on its own.
The Need for Medical Device Regulation
What was clearly needed, according to many, was national regulation of the medical device industry. Besides being subjected to enforcement actions against products that had already tragically demonstrated their danger to people, medical devices were officially defined as drugs. Calling a medical device a drug, claimed a U.S. senator from Missouri at the time, was like "calling a sheep's tail a leg." Legislation was eventually introduced to modernize the 1906 act. The contentious Senate debate that led up to enactment of the Federal Food, Drug, and Cosmetic Act (FD&C Act) of 1938 had much to do with the definition of a medical device being added to the law.
Nevertheless, from 1938 until the early 1960s, devices were subject only to policing by the FDA. The agency determined whether a device was safe and effective. If not, the agency could bring charges in the courts only against products or materials that were found to be defective, unsafe, filthy, or produced in unsanitary conditions (adulterated), or against statements, designs, or labeling that was false or misleading (misbranded). There was, however, no requirement for pre-market testing, review, or approval.
The FDA's enforcement resources would be strained to the limit over the next 25 years as the agency attempted to deal with such widely distributed quack machines and gadgets such as Ruth B. Drown's Radio Therapeutic Instrument.
Proponents of this device claimed it could cure ailments ranging from a simple fungus growth to a potentially fatal kidney malfunction. Worse yet, when patients' illnesses became too debilitating for them to make the trip to the doctor's office for treatment, they were told they could be treated by remote control.
"That's what's wonderful about the Drown machine," FDA court transcripts quote one doctor as saying. "It's just as effective when the patient is miles away, as when he or she's here." Court documents revealed that four years after one woman faithfully used the radio instrument, she died of the very cancer that Ruth B. Drown's machine, in truth, was incapable of diagnosing or curing.
Such devices were successfully removed from the market. These actions, however, consumed such a large amount of the agency's resources that consideration was given to enactment of additional legislation to further strengthen the FDA's authority.
In 1962, President John F. Kennedy proposed changes to the way medical devices entered the market. Extensive congressional hearings were held on proposals to revise the FD&C Act in a number of different ways, including a requirement that medical devices be regulated comparably to, but separately from, new drugs. There were signs that progress was being made on the proposals.
A few months later, however, news came that thousands of European babies whose mothers took the sedative thalidomide had been born with terrible deformities. The issue of medical devices was then set aside so that health officials could focus on the tragedy.
Congress considered a comparable device law when it passed the 1962 drug amendments. The companion bill, however, to require pre-market approval of new medical devices under the same type of system applied to new drugs was deleted from that final legislation.
The Medical Device Amendments of 1976
During the 1960s and into the 1970s, the FDA's attention turned to the wide range of life-saving medical devices. The agency devoted considerably more effort to ensuring the safety and effectiveness of these new devices, while still trying to protect the public against the fraudulent ones.
The Cooper Committee--chaired by Theodore Cooper, M.D., then director of the National Heart and Lung Institute--was organized in 1970 specifically to study medical devices as part of President Richard M. Nixon's endorsement of medical device legislation. The committee recommended that any new legislation be specifically targeted to the device industry, because devices presented entirely different issues from drugs. It also suggested that different classifications for medical devices be created, which would tailor the regulatory controls to the risks involved.
Because Congress could not initially agree on the draft legislation for medical devices, the FDA forced the issue and, on its own initiative, took the committee's recommendations by taking inventory of all medical devices being used and then classifying them according to their potential risks.
"That finally got the attention of the House as well as the Senate," said Peter Barton Hutt, who served as chief counsel for the FDA between 1971 and 1974, "and they both began to show renewed interest in late 1974."
The 1976 Medical Device Amendments Become Law
While the Cooper Committee recommendations were being debated in Congress during 1972 and 1973, pacemaker failures were reported. And in 1975, hearings took place on problems that had been reported with the Dalkon Shield intrauterine device, which caused thousands of reported injuries. Those two incidents helped underscore the need for the Medical Device Amendments, enacted in 1976.
President Gerald R. Ford, in signing the law, said, "The Medical Device Amendments of 1976 eliminate the deficiencies that accorded FDA 'horse and buggy' authority to deal with 'laser age' problems." He added, "I welcome this legislation and commend the FDA, who identified the need, cooperated in its development, and finally, will be entrusted with its enforcement."
The 1976 amendments defined devices similarly to drugs, but noted that drugs cause a chemical reaction in the body, whereas devices do not. They called for all devices to be divided into classes, with varying amounts of control required in each one.
Tongue depressors, for example, would fall under general controls of the types already existing (Class I); wheelchairs would be subjected to performance standards when general controls were deemed insufficient to assure product safety and effectiveness (Class II); while artificial hearts would be required to go through pre-market approval (Class III). The agency's first device performance standard was developed for impact-resistant lenses in eyeglasses and sunglasses.
The final provisions of the 1976 amendments closely resemble the Cooper Committee recommendations. In addition to the medical device inventory and classification requirements, Class III device manufacturers were required to notify the FDA prior to marketing. New devices that were substantially equivalent to pre-1976 devices could be marketed immediately, subject to any existing or future requirements for that type of device.
Good Manufacturing Practice (GMP) regulations also were authorized at that time. These are a set of procedures to ensure that devices are manufactured to be safe and effective through quality design, manufacture, labeling, testing, storage, and distribution.
"The development of the GMP regulation included significant interaction with the medical device industry, which resulted in a set of requirements that stood the test of time for 20 years," recalls David M. Link, former director of the FDA's then Bureau of Medical Devices, at a 20th anniversary of the medical device law. Link, who served as bureau director between 1974 and 1980, said it is a gratifying reflection that "a number of the processes initiated in the late 70s are still in place."
During the 1980s, spectacular growth began to occur in the related field of medical diagnostic devices, which aid in the detection of diseases and other conditions, such as pregnancy.
"It was an exciting time to be in FDA and the bureau," says Victor Zafra, former acting director of the Bureau of Medical Devices from 1980 to 1982, "because many of the initial policies and regulations were developed at that time." Zafra remembers approval of the first monoclonal antibody in vitro diagnostic test kit, as well as extended-wear soft contact lenses.
With the development of electronic technology came a host of new products and, with them, potential harmful radiation exposure. But the tools to solve their potential dangers, as recognized by the act--training, research, and state collaboration--were perceived as less enforcement-oriented than the traditional FDA approach to regulation. Responsibility for radiation product activities fell under the agency's then Bureau of Radiological Health, which was combined in 1982 with the Bureau of Medical Devices and renamed the CDRH.
"Consequently, there was the challenge of preserving these 'softer' radiation programs and at the same time building a credible compliance program in the new center," says John C. Villforth, who served as director of the CDRH from 1982 to 1990. The most important challenge facing the new organization, he emphasized, was the merging of the two bureaus into a single center.
"Both bureaus had a similar culture in that they were involved with 'things' as opposed to foods or drugs," he said, "and so there was a reasonable fit in the disciplines--primarily physical sciences and engineering--that were needed to regulate the combined programs."
But Mark Barnett, the CDRH's assistant director for education and communications since its inception in 1982, says it isn't just the emphasis on physics and engineering that distinguishes medical devices and radiological equipment from drugs.
"The safety of most medical devices depends to a large degree on their being used properly," he says. "That's true in the case of a surgeon implanting a prosthetic device in a patient's body, an anesthesiologist operating a complex gas delivery machine, or a diabetic patient using a blood glucose monitor at home. And so, with devices," he adds, "an important part of our job is to educate health care practitioners and patients about safe use."
Villforth adds, "I believe the melding of the talents of both bureaus into the combined center was responsible for the success that CDRH has maintained over the years."
The Medical Device Amendments also gave the FDA authority to deal with the notification, repair, replacement, and refund of defective devices, and the agency was authorized to ban any device that presents a substantial deception or substantial unreasonable risk of injury or illness. Thus, the final law greatly strengthened the FDA's authority to regulate medical devices, but retained the fundamental concept of the Cooper Committee report that regulation should be carefully tailored to the type of device involved.
More Medical Device Milestones
The Safe Medical Devices Act (SMDA) was passed in 1990, and represents the first reform of medical device law since the 1976 amendments. This law modified the amendments to give the public greater protection against dangerous medical devices.
Specifically, the SMDA requires nursing homes, hospitals, and other health care facilities that use medical devices to report to the FDA incidents suggesting that a medical device probably caused or contributed to a patient's death, serious illness, or serious injury. Manufacturers are now required to conduct post-market surveillance on permanently implanted devices whose failure might cause serious harm or death, and to establish methods for tracing and locating patients who depend on such devices. The SMDA authorizes the FDA to order device product recalls and other actions.
"Looking back to the time that I was center director, mid '91 through '92," recalls James S. Benson, a former CDRH director, "I see a center that was severely challenged. We faced implementation of SMDA under tremendous congressional pressure. We faced a very difficult process, exacerbated by enormous press interest, of trying to figure out how to deal with breast implants."
"At the time, we were trying to find resources that would allow the device law to be fully implemented," Benson says.
In 1992, Congress passed the Mammography Quality Standards Act (MQSA). The act requires all mammography facilities in the United States to be accredited and certified as meeting quality standards as of Oct. 1, 1994. The goal of the MQSA is to enhance the detection of breast disease through high-quality mammography services. After initial certification, facilities must pass annual inspections by federal or state inspectors.
New programs like this "had come the center's way," says D. Bruce Burlington, M.D., the CDRH director from 1993 to 1999. "Organizing and executing to successfully reinvent key center processes, write numerous rules and guidelines at a record rate, and keep the usual work moving on time," he says, "was only possible with the teamwork and high performance that have always made CDRH a great place to work." By October 2002, the FDA reported it had certified 9,306 mammography facilities and conducted more than 96,000 annual and biannual inspections.
The Medical Device User Fee and Stabilization Act (MDUFSA) of 2005 is the latest major medical device law to be enacted. The MDUFSA amends the user-fee system created by the original Medical Device User Fee and Modernization Act of 2002, which allows the FDA to charge a fee for medical device product reviews. The agency uses these funds to hire staff and develop better systems to support effective and timely product reviews, to enact needed regulatory reforms, and to ensure that reprocessed devices are as safe and effective as the original devices. The aim of the legislation is to bring safe and effective devices to the public sooner.
"Timely decisions based on sound science" continues to be the center's goal in bringing new products to the market, says David W. Feigal, M.D., M.P.H., who served as CDRH director from 1999 to 2004. He cited some of the center's accomplishments as the development of approaches with the CDRH team to deal with emerging problems such as reuse of single-use devices, regulation of "home brew" genetic tests, revitalization of the radiological health programs, and the process of recruiting the next generation of CDRH leadership.
30 Years of Medical Device Regulation and Beyond
Two major milestones in the FDA's regulation of medical devices occurred when devices were first brought under federal regulatory control in 1938, and when they were first subjected to pre-market review in 1976. On both occasions, the agency sought to balance the need to protect the public from adulteration and misbranding of medical devices against the need to foster the development of innovative new life-saving medical devices.
Today, among other activities, the CDRH devotes a great deal of time to working cooperatively with other agency centers to resolve issues dealing with combination products, such as drugs that are also considered devices; miniature devices (nanotechnology) that will provide less-invasive surgery, which ultimately will result in quicker recovery times for patients; and FDA training on new technology as it develops.
Because of the agency's timely, science-based decisions, millions of Americans get the medical products they need and can be assured of their safety and effectiveness. The FDA's scientific investment brings tangible public health benefits, such as the development of state-of-the-art diagnostic techniques based on genetic mapping. This, says CDRH Director Daniel G. Schultz, M.D., makes it possible for faster and much more accurate identification of people who are at high risk for diseases such as cancer, or who are prone to experience certain adverse drug reactions.
"When I think about the future of our medical device program," Schultz says, "two words come to mind: 'excitement' and 'challenge.' The excitement comes from the tremendous progress the scientific community is making in unraveling the body's secrets at a genetic and molecular level, and from the promise that these discoveries will translate into life-saving and life-enhancing products."
The challenge, he adds, "will be to regulate these new products so as to assure their safety and effectiveness while at the same time assuring that we don't impede medical progress."