Pelvic Organ Prolapse (POP)
On this page:
- What is Pelvic Organ Prolapse?
- What are the Treatment Options for Pelvic Organ Prolapse?
- What Should I Do if Surgical Mesh Was Used to Repair My Pelvic Organ Prolapse Transvaginally?
What is Pelvic Organ Prolapse?
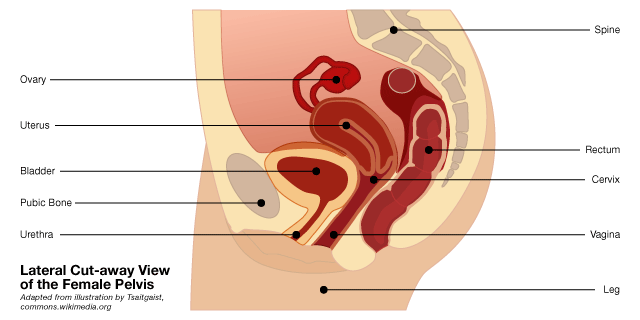
Pelvic organ prolapse (POP) occurs when the tissue and muscles of the pelvic floor no longer support the pelvic organs resulting in the drop (prolapse) of the pelvic organs from their normal position. The pelvic organs include the vagina, cervix, uterus, bladder, urethra, and rectum. The bladder is the most commonly involved organ in pelvic organ prolapse.
Supporting muscles and tissue of the pelvic floor may become torn or stretched because of labor or childbirth or may weaken with age. Other risk factors for POP include: genetic predisposition, connective tissue disorder, obesity and frequent constipation.
Many women have some degree of POP, although not all women have symptoms. Women who have symptoms may experience pelvic discomfort or pain, pressure and other symptoms including:
- bulge of tissue or organs that protrudes to or past the vaginal opening
- leakage of urine (urinary incontinence)
- sexual difficulties
It is important for women to consult with their health care provider for proper diagnosis of POP.
What are the Treatment Options for Pelvic Organ Prolapse?
After obtaining a detailed medical history and completing a thorough physical exam, your health care provider can recommend treatment options for your pelvic organ prolapse (POP). Nonsurgical or surgical treatment is usually effective but it may not completely solve all symptoms associated with POP such as pelvic pain or pressure.
NONSURGICAL TREATMENT OPTIONS
Examples of nonsurgical treatment options for POP include:
- Pelvic Floor Exercises: A type of exercise to strengthen the pelvic floor by contracting and relaxing the muscles that surround the opening of the urethra, vagina, and rectum. The exercises are commonly referred to as Kegels.
- Pessary: A removable device that is inserted into the vagina to support the pelvic organ(s) that have prolapsed.
SURGICAL TREATMENT OPTIONS
Not every woman with POP will need surgery. Surgery may be recommended for women with significant discomfort or pain from POP that impairs their quality of life. If surgery is recommended, factors to consider include:
- which organ(s) have prolapsed
- severity of prolapse
- desire for future children
- age
- sexual activity
- severity of symptoms
Surgery to repair POP can be done through either the vagina or abdomen, using stitches (sutures) alone or with the addition of surgical mesh. Surgical options include restoring the normal position of the vagina, repairing the tissue around the vagina, permanently closing the vaginal canal with or without removing the uterus (colpocleiesis).
It is also possible that women with POP may experience problems with urine leakage (incontinence). During surgery, a procedure to prevent or decrease urine leakage (which may also use surgical mesh) may be performed.
The FDA identified serious complications associated with the use of urogynecologic surgical mesh. Detailed information on its safety and effectiveness can be found in: Urogynecologic Surgical Mesh: UPDATE ON THE SAFETY AND EFFECTIVENESS OF Transvaginal PLACEMENT for Pelvic Organ Prolapse.
What Should I Do if Surgical Mesh Was Used to Repair My Pelvic Organ Prolapse Transvaginally?
If you had surgery with mesh to repair your POP transvaginally, you should:
- Continue with your annual and other routine check-ups and follow-up care. There is no need to take additional action if you are satisfied with your surgery and are not having complications or symptoms.
- Notify your health care provider if you have complications or symptoms develop, such as persistent vaginal bleeding or discharge, pelvic or groin pain, or pain during sexual intercourse.
- Let your health care provider know you have surgical mesh, especially if you plan to have another surgery or other medical procedures.
- Talk to your health care provider about any questions you may have.
- Submit a voluntary report about any problems experienced with surgical mesh for repair of pelvic organ prolapse through Medwatch, the FDA Safety Information and Adverse Event Reporting program.
If you have had transvaginal POP surgery but do not know whether your surgeon used mesh, ask your surgeon at your next scheduled visit.