Towards Longer-Acting Factor VIII Products with Better Purity
Andrey Sarafanov, Ph.D.
Office of Tissues and Advanced Therapies
Division of Plasma Protein Therapeutics
Hemostasis Branch
Biosketch
Andrey G Sarafanov, PhD is a principal investigator in the Hemostasis Branch of OTAT/DPPT. The general area of his expertise is biochemistry and molecular biology. In his regulatory work, Dr. Sarafanov reviews applications for plasma-derived and recombinant therapeutic proteins for treating deficiencies in blood coagulation that cause excessive bleeding. Dr. Sarafanov studies the structure, functions, and mechanisms of circulatory clearance of the blood coagulation factor VIII (FVIII) and von Willebrand factor (vWF). This study is relevant to the regulation and generation of new longer-acting FVIII and vWF products designed to improve treatment of patients with deficiencies in these factors (Hemophilia A and von Willebrand disease). Dr. Sarafanov received his PhD from the Engelhard Institute of Molecular Biology Russian Academy of Sciences (Moscow) in 1998. From 1999-2008, he worked in the Holland Laboratory of the American Red Cross, University of Maryland, and the Armed Forces Institute of Pathology. In 2008, Dr. Sarafanov joined CBER/OBRR, where his lab moved from into OTAT/DPPT in 2016.
General Overview
Hemophilia A is a bleeding disorder caused by congenital deficiency of factor VIII (FVIII), a protein found in blood. The disease is sex-linked and occurs in one in ~5,000 males but is very rare in women. The treatment involves infusions of an FVIII concentrate, which compensates for its deficiency. The therapeutic FVIII is either purified from human blood or generated in cell culture using recombinant DNA. FVIII obtained from blood carries a risk of transmitting blood-borne infections to the patient; therefore, some physicians prefer to use recombinant FVIII. However, a number of other problems are still associated with the treatment. These are (i) complexity of the treatment, requiring up to three-four infusions of FVIII each week, (ii) high cost (up to $500,000 per year), and (iii) development of FVIII inhibitors (anti-FVIII antibodies) in ~30% of patients that makes the treatment ineffective. In part, the formation of FVIII inhibitors (immune response) can be related to the presence of FVIII forms with altered structure and properties (defined as impurities), which appear during the manufacturing process. The treatment would be more efficient if the therapeutic FVIII lasts longer in circulation and has higher purity.
Review of therapeutic FVIII products is a responsibility of the Division of Plasma Protein Therapeutics. To better understand such products, we study how the structure of FVIII affects the rate at which it is physiologically removed (cleared) from circulation. Specifically, we investigate how FVIII interacts with particular liver receptors that remove it from the blood flow. We also characterize the purity of FVIII products as a patient-safety factor and develop methods to control specific product-related impurities from those products. Our experimental approaches include using recombinant DNA technology to generate proteins in cell culture, testing protein interactions, developing analytical methods and using cell culture and animal (mice) models. Our studies help to understand the mechanisms of FVIII clearance from blood and improve purity of FVIII concentrates. This knowledge facilitates regulation of FVIII products, in particular, those designed to have prolonged therapeutic effect. Altogether, this improves safety and efficacy of FVIII products, and thus, treatment of Hemophilia A.
Scientific Overview
Congenital deficiency in blood coagulation factor VIII (FVIII) results in a blood coagulation disorder (Hemophilia A) that is treated with infusions of plasma-derived (pdFVIII) or recombinant (rFVIII) FVIII concentrates. The hemophilia community hopes for improvements in FVIII products, in particular, those with therapeutic effects that are prolonged enough to reduce the infusion frequency, and possibly the cost of treatment. Therefore, manufacturers modify structures of the rFVIII to make it last longer in the circulation. Such designs require understanding mechanisms of FVIII clearance from circulation that our studies are aimed to elucidate. We believe that our studies will facilitate regulation of current products and generation of new longer-acting FVIII products for improved management of Hemophilia A.
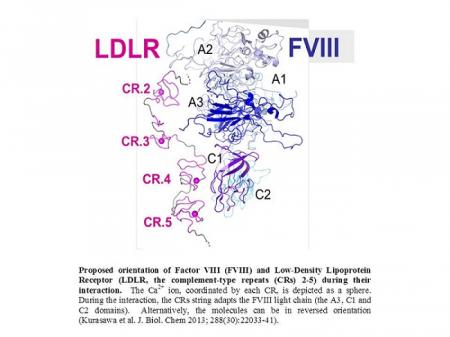
The life-time of FVIII in circulation depends on various factors which involve interactions of FVIII with von Willebrand Factor (vWF, a carrier of FVIII in blood) and hepatic clearance receptors. Among these receptors, the major role in FVIII clearance belongs to the low-density lipoprotein-related protein 1 (LRP1), which catabolizes FVIII and the FVIII/vWF complex from circulation; and the low-density lipoprotein receptor (LDLR), which acts in concert with LRP1 in catabolizing free FVIII. We investigate respective molecular interactions using in silico, in vitro, and in vivo models. Our methodology includes site-directed mutagenesis, hydrogen-deuterium exchange/mass-spectrometry, circular dichroism, surface plasmon resonance, cell culture and animal models, etc. Upon understanding respective molecular mechanisms, we plan to suggest modifications of the proteins structure, so the modified FVIII and vWF would have reduced binding to LRP1 (LDLR) and prolonged half-life(s) in a murine model. Such proteins can be models of a longer-acting therapeutic FVIII and vWF. Notably, longer-acting vWF can be used for better treatment of patients with deficiency in vWF (vWF Disease).
We also characterize FVIII products for content and nature of functionally/structurally compromised forms of FVIII, representing product-related impurities which pose a concern for products efficacy. Upon treatment with FVIII products, ~30% of the patients develop FVIII inhibitors (anti-FVIII antibodies), which neutralize the FVIII function and make the treatment ineffective. Many studies indicate that the risk of inhibitor formation when using rFVIII is higher than that of pdFVIII. This correlates with apparently higher content of structurally altered protein in rFVIII products, reflected by more than 3-fold variations in the specific activity, shown in previous studies and, for selected products, available from the prescribing information (https://dailymed.nlm.nih.gov/). The structurally altered forms of FVIII, such as truncated, denatured, aggregated, misfolded, those having incomplete or changed post-translational modifications etc., can be immunogenic and promote formation of FVIII inhibitors. We perform research to characterize and control such proteins (product-related impurities) in rFVIII products to achieve their higher purity, and thus, efficacy for the improved treatment of Hemophilia A.
Important Links
-
ORCID ID: https://orcid.org/0000-0001-6124-9713
Publications
- Int J Mol Sci 2023 May 11;24(10):8584
Plasma clearance of coagulation factor VIII and extension of its half-life for the therapy of hemophilia A: a critical review of the current state of research and practice.
Sarafanov AG - J Thromb Haemost 2022 Oct;20(10):2255-69
Characterization of interaction between blood coagulation factor VIII and LRP1 suggests dynamic binding by alternating complex contacts.
Chun H, Kurasawa JH, Olivares P, Marakasova ES, Shestopal SA, Hassink GU, Karnaukhova E, Migliorini M, Obi JO, Smith AK, Wintrode PL, Durai P, Park K, Deredge D, Strickland DK, Sarafanov AG - Int J Mol Sci 2022 Jul 23;23(15):8134
Isolated variable domains of an antibody can assemble on blood coagulation factor VIII into a functional Fv-like complex.
Shestopal SA, Parunov LA, Olivares P, Chun H, Ovanesov MV, Pettersson JR, Sarafanov AG - J Biol Chem 2021 Jul;297(1):100842
Molecular chaperone RAP interacts with LRP1 in a dynamic bivalent mode and enhances folding of ligand-binding regions of other LDLR family receptors.
Marakasova E, Olivares P, Karnaukhova E, Chun H, Hernandez NE, Kurasawa JH, Hassink GU, Shestopal SA, Strickland DK, Sarafanov AG - J Thromb Haemost 2021 Apr;19(4):954-66
Characterization of protein unable to bind von Willebrand factor in recombinant factor VIII products.
Chun H, Pettersson JR, Shestopal SA, Wu WW, Marakasova ES, Olivares P, Surov SS, Ovanesov MV, Shen RF, Sarafanov AG - J Thromb Haemost 2017 Apr;15(4):709-20
Expression and characterization of a codon-optimized blood coagulation factor VIII.
Shestopal SA, Hao JJ, Karnaukhova E, Liang Y, Ovanesov MV, Lin M, Kurasawa JH, Lee TK, McVey JH, Sarafanov AG - Haemophilia 2016 Sep;22(5):780-9
Optimization of the thrombin generation test components to measure potency of factor VIII concentrates.
Jha NK, Shestopal SA, Gourley MJ, Woodle SA, Liang Y, Sarafanov AG, Weinstein M, Ovanesov MV - Biochim Biophys Acta 2016 Jun;1858(6):1216-27
Hysteresis-like binding of coagulation factors X/Xa to procoagulant activated platelets and phospholipids results from multistep association and membrane-dependent multimerization.
Podoplelova NA, Sveshnikova AN, Kurasawa JH, Sarafanov AG, Chambost H, Vasil'ev SA, Demina IA, Ataullakhanov FI, Alessi MC, Panteleev MA - Biochemistry 2015 Jan;54(2):481-9
Cluster III of low-density lipoprotein receptor-related protein 1 binds activated blood coagulation factor VIII.
Kurasawa JH, Shestopal SA, Woodle SA, Ovanesov MV, Lee TK, Sarafanov AG