Impact Story: Determining the Clinical Benefit of Treatment Beyond Progression with Immune Checkpoint Inhibitors
CDER researchers are evaluating whether it is clinically beneficial to treat cancer patients with checkpoint inhibitors if their tumors do not immediately shrink in response to these drugs.
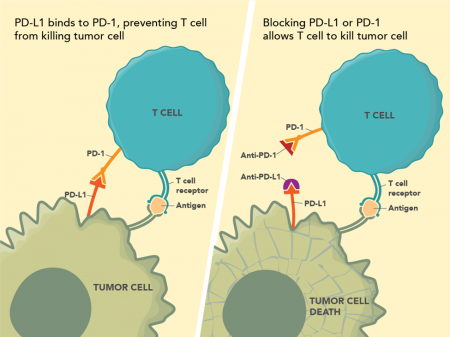
In 2018, James Allison and Tasuku Honjo won the Nobel Prize in Physiology or Medicine for their work leading to the development of immune checkpoint inhibitors, a type of cancer drug that blocks certain proteins made by some types of immune cells.1 Their breakthrough underscores how the ability to manipulate the human immune system has transformed cancer treatment (Figure 1). These drugs have led to dramatic responses in several advanced cancers, including metastatic melanoma, lung cancer, kidney cancer, bladder cancer, and head and neck cancers.
However, in some patients, these drugs do not shrink the tumors or reduce tumor growth, and these patients may need to undergo alternative treatments. Moreover, approximately 4 percent of patients with solid tumors treated with immune checkpoint inhibitors demonstrate “pseudoprogression,” meaning that imaging data show initial tumor growth followed by tumor shrinkage.2
Pseudoprogression complicates decision-making for clinicians who treat patients and for regulators who specify indications for these drugs. Some oncologists continue to treat patients even when imaging data indicates that the tumor has progressed. This is called “treatment beyond progression.” However, the clinical benefit of treatment beyond progression is unknown, and the approach carries some risks:
- Delay of administration of an alternative, potentially effective therapy
- Safety issues associated with continuing treatment with immune checkpoint inhibitors, such as immune-related adverse events
CDER Analysis of Pooled Data
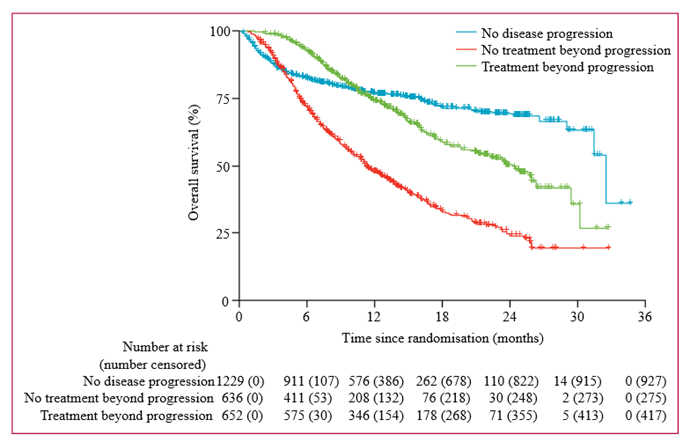
To address the question of whether treatment beyond progression has clinical benefit, CDER researchers pooled data from eight melanoma trials submitted to FDA. The analysis included approximately 2,600 patients who were treated with the checkpoint inhibitors pembrolizumab or nivolumab. In about half of the patients treated with these drugs, the melanoma continued to progress. In this group, about 600 patients received treatment beyond progression and approximately the same number of patients did not (although many of these patients received other types of treatment). The group who received treatment beyond progression demonstrated a longer median overall survival than the group who did not (24.2 months compared with 11.2 months; Figure 2).
The CDER researchers could not draw definitive conclusions about a survival benefit of treatment beyond progression, because there may have been important differences in known and unknown prognostic factors (Box 1) among patients who received treatment beyond progression and those who did not, such as the cancer location and the patients’ level of functioning. The researchers also found no difference in the incidence of adverse events (including immune-related adverse effects) between the two groups.
Based on the results of the analysis of both survival outcomes and toxicity associated with immune checkpoint inhibitors, the researchers suggested that before deciding whether to recommend treatment beyond progression, physicians should consider the extent of the cancer’s progression and the patient’s status.
The role of prognostic factors in the pooled analysis
A prognostic factor is something that affects a patient’s overall outcome for a disease regardless of an intervention. Beaver et al. hypothesized that the patients treated beyond progression in the trials included in the FDA pooled analysis may have been selected by the physicians because of positive prognostic factors, such as3:
- Absence of signs and symptoms
- Laboratory values
- Stable or improved ECOG performance score, which is a scale used to assess how a patient’s disease is progressing by determining how the disease affects the patient’s daily living abilities
- Absence of rapid disease progression that requires urgent medical attention
The possibility that different groups of patients have different prognostic factors confounds attempts of the analysis to conclude whether treatment beyond progression led to a better outcome for these patients.
Future Directions
Figure 2: Summary of Pooled Overall Survival Analysis
This figure summarizes the results of a study from Beaver et. al., where the group of patients who received treatment beyond progression demonstrated a longer median overall survival than the group who did not. Source: Beaver et al. 2018.
Several new areas of research will likely drive progress in understanding whether treatment beyond progression has clinical benefit. For example, the scientific community is working to develop new standardized approaches for measuring tumors in patients treated with immune checkpoint inhibitors—a modified version of Response Evaluation Criteria in Solid Tumors for immune-based therapeutics (iRECIST). This approach could improve our ability to distinguish pseudoprogression from true progression. Radiomics, the application of artificial intelligence methods to quantitatively analyze tumor images, and/or the use of liquid biopsies may also provide us with new insight.
Two groups of recently developed drugs (PD1/PD-L1 and CTLA-4 inhibitors) are monoclonal antibodies that bind to immune checkpoint proteins, allowing cells to recognize and kill cancer cells.
How does this pooled analysis advance regulatory science?
Although this pooled analysis of clinical trials submitted to FDA by developers of checkpoint inhibitors did not provide definitive data on the clinical benefit of treatment beyond progression, it did suggest that treatment beyond progression was not associated with a large increase in adverse events. The authors recommended that patient selection criteria be pre-specified in all clinical protocols and that patients receive informed consent documents detailing what is known about treatment beyond progression. FDA has not recommended the continuation of treatment beyond progression in any product labeling. Deciding whether to keep a patient on immunotherapy in clinical practice should continue to be based on factors such as the extent of disease progression and the physician’s assessment of the patient’s status.
Selected Publications
- Yeager A, K Grens, Oct. 1, 2018, James Allison and Tasuku Nonjo Win Nobel Prize, The Scientist.
- Chiou, VL, M Burotto, 2015, Pseudoprogression and Immune-Related Response in Solid Tumors, Journal of Clinical Oncology 33 (31): 3541-3543.
- Beaver, JA, M Hazarika, F Mulkey, S Mushti, H Chen, K He, et al., 2018, Patients with Melanoma Treated with an Anti-PD-1 Antibody Beyond RECIST Progression: A US Food and Drug Administration Pooled Analysis, Lancet Oncology 19 (2): 229-239.
Eisenhauer, EA, P Therasse, J Bogaerts, LH Schwartz, D Sargent, R Ford, et al., 2009, New Response Evaluation Criteria in Solid Tumors: Revised RECIST Guideline (Version 1.1), European Journal of Cancer, 45 (2): 228-2247.
Seymour, L, J Bogaerts, A Perrone, R Ford, LH Schwartz, S Mandrekar, et al., 2017, iRECIST: Guidelines for Response Criteria for Use in Trials Testing Immunotherapeutics, Lancet Oncology, 18 (3): e143-e152.
Wolchok, JD, A Hoos, S O’Day, JS Weber, O Hamid, C Lebbé, et al., 2009, Guidelines for the Evaluation of Immune Therapy Activity in Solid Tumors: Immune-Related Response Criteria, Clinical Cancer Research, 15 (23): 7412-7420.
Related Guidance
Guidance for Industry: Clinical Trial Endpoints for the Approval of Cancer Drugs and Biologics (PDF – 228 KB)