Drug Trials Snapshots: IDHIFA
HOW TO USE THIS SNAPSHOT
The information provided in Snapshots highlights who participated in the clinical trials that supported the FDA approval of this drug, and whether there were differences among sex, race, and age groups. The “MORE INFO” bar shows more detailed, technical content for each section. The Snapshot is intended as one tool for consumers to use when discussing the risks and benefits of the drugs.
LIMITATIONS OF THIS SNAPSHOT:
Do not rely on Snapshots to make decisions regarding medical care. Always speak to your health provider about the risks and benefits of a drug. Refer to IDHIFA Prescribing Information for complete information.
IDHIFA (enasidenib)
eyed-HEE-fuh
Celgene
Approval date: August 1, 2017
DRUG TRIALS SNAPSHOT SUMMARY:
What is the drug for?
IDHIFA is used to treat adults with acute myeloid leukemia (AML) that have a mutation in a gene called IDH2 and whose disease has come back or has not improved after previous treatment(s).
AML is a rapidly progressing cancer that forms in the bone marrow and results in an increased number of white blood cells in the bloodstream.
How is this drug used?
IDHIFA is a tablet. One or two tablets (total of 100 mg) are taken once a day.
What are the benefits of this drug?
19 percent of the 199 patients who received IDHIFA experienced no evidence of disease and full recovery of blood counts after treatment (complete remission) which lasted about 8 months.
Of the 157 patients who required transfusions of blood or platelets due to AML at the start of the trial, 34 percent no longer required transfusions after treatment with IDHIFA.
What are the benefits of this drug (results of trials used to assess efficacy)?
The table below summarizes efficacy results established on the basis of the rate of complete response (CR)/complete response with partial hematologic recovery (CRh), the duration of CR/CRh, and the rate of conversion from transfusion dependence to transfusion independence.
Table 2: Efficacy Results in Patients with Relapsed or Refractory Acute Myeloid Leukemia (AML)
| Endpoint | IDHIFA (100 mg daily) N=199 |
|---|---|
| CRa n (%) | 37 (19) |
| 95% CI | (13, 25) |
| Median DORb (months) | 8.2 |
| 95% CI | (4.7, 19.4) |
| CRhc n (%) | 9 (4) |
| 95% CI | (2, 8) |
| Median DOR (months) | 9.6 |
| 95% CI | (0.7, NA) |
| CR/CRh n (%) | 46 (23) |
| 95% CI | (18, 30) |
| Median DOR (months) | 8.2 |
| 95% CI | (4.3, 19.4) |
CI: confidence interval, NA: not available
a CR (complete remission) was defined as <5% of="" blasts="" in="" the="" bone="" marrow,="" no="" evidence="" of="" disease,="" and="" full="" recovery="" of="" peripheral="" blood="" counts="" (platelets="">100,000/microliter and absolute neutrophil counts [ANC] >1,000/microliter).
b DOR (duration of response) was defined as time since first response of CR or CRh to relapse or death, whichever is earlier.
c CRh (complete remission with partial hematological recovery) was defined as <5% of="" blasts="" in="" the="" bone="" marrow,="" no="" evidence="" of="" disease,="" and="" partial="" recovery="" of="" peripheral="" blood="" counts="" (platelets="">50,000/microliter and ANC >500/microliter).
IDHIFA Prescribing Information
Were there any differences in how well the drug worked in clinical trials among sex, race and age?
- Sex: IDHIFA worked similarly in men and women.
- Race: Most of the patients were White. Differences in how well the drug worked among races could not be determined because of the small number of patients in other races.
- Age: IDHIFA worked similarly in patients younger and older than 65 years of age.
Were there any differences in how well the drug worked in clinical trials among sex, race, and age groups?
The table below summarizes efficacy results by demographic subgroups. These analyses were exploratory and therefore should be interpreted with caution.
Table 3. Subgroup Analyses of Complete Response Rate by Sex, Race, Age, and Region
| IDHIFA (N=199) | ||
|---|---|---|
| Complete Response Rate n/N (%) | 95% CI | |
| Sex | ||
| Men | 20/103 (19.4) | 12.3, 28.3 |
| Women | 17/96 (17.7) | 10.7, 26.8 |
| Race | ||
| White | 27/153 (17.7) | 12.0, 24.6 |
| Not provided | 7/25 (21.9) | 9.3, 40.0 |
| Age | ||
| ≤ 65 years | 7/76 (7.4) | 3.8, 18.1 |
| >65 years | 30/123 (24.4) | 17.1, 33.0 |
| Region | ||
| US | 28/166 (16.9) | 11.5, 23.5 |
| France | 9/33 (27.3) | 13.3, 45.5 |
FDA review
What are the possible side effects?
IDHIFA may cause serious and life threating effect called differentiation syndrome.
Common side effects of IDHIFA are nausea, vomiting, diarrhea, increased bilirubin level and decreased appetite.
What are the possible side effects (results of trials used to assess safety)?
The tables below summarize adverse reactions and laboratory abnormalities in the clinical trial.
Table 4. Adverse Reactions Reported in ≥10% (Any Grade) or ≥3% (Grade 3-5) of Patients with Relapsed or Refractory AML
| IDHIFA N=214 |
||
|---|---|---|
| Body System Adverse Reaction |
All Grades N=214 n (%) |
≥Grade 3 N=214 n (%) |
| Gastrointestinal Disorders a | ||
| Nausea | 107 (50) | 11 (5) |
| Diarrhea | 91 (43) | 17 (8) |
| Vomiting | 73 (34) | 4 (2) |
| Metabolism and Nutrition Disorders | ||
| Decreased appetite | 73 (34) | 9 (4) |
| Tumor lysis syndrome b | 13 (6) | 12 (6) |
| Blood and Lymphatic System Disorders | ||
| Differentiation syndrome c | 29 (14) | 15 (7) |
| Noninfectious leukocytosis | 26 (12) | 12 (6) |
| Nervous System Disorders | ||
| Dysgeusia | 25 (12) | 0 (0) |
Gastrointestinal disorders observed with IDHIFA treatment can be associated with other commonly reported events such as abdominal pain, and weight decreased.
b Tumor lysis syndrome observed with IDHIFA treatment can be associated with commonly reported uric acid increased
c Differentiation syndrome can be associated with other commonly reported events such as respiratory failure, dyspnea, hypoxia, unexplained pyrexia, peripheral edema, rash, or renal insufficiency.
IDHIFA Prescribing Information
Table 5. Most Common (≥20%) New or Worsening Laboratory Abnormalities Reported in Patients with Relapsed or Refractory AML
| IDHIFA N=214 |
||
|---|---|---|
| Parameter a | All Grades (%) |
Grade ≥3 (%) |
| Total bilirubin increased | 81 | 15 |
| Calcium decreased | 74 | 8 |
| Potassium decreased | 41 | 15 |
| Phosphorus decreased | 27 | 8 |
a Includes abnormalities occurring up to 28 days after last IDHIFA dose, if new or worsened by at least one grade from baseline, or if baseline was unknown. The denominator varies based on data collected for each parameter (N=213 except phosphorous N=209).
IDHIFA Prescribing Information
Were there any differences in side effects among sex, race and age?
- Sex: The occurrence of side effects was similar in men and women.
- Race: Most of the patients were White. Differences in the occurrence of side effects among races could not be determined because of the small number of patients in other races.
- Age: The occurrence of side effects was similar in patients younger and older than 65 years of age.
Were there any differences in side effects of the clinical trials among sex, race, and age groups?
Tables below summarize adverse events during the clinical trials by sex, age and race subgroup.
Table 6. Subgroup Analyses of Adverse Events
| Subgroups | IDHIFA N=214 | ||
|---|---|---|---|
| TEAE x (%) |
SAE x (%) |
||
| All Patients | 214 (100) | 165 (77) | |
| Sex, (n) | |||
| Men (109) | 109 (100) | 84 (77) | |
| Women (105) | 105 (100) | 81 (77) | |
| Age Group (n) | |||
| <65 years, | 85 (100) | 72 (85) | |
| >=65 years, (129) | 129 (100) | 93 (72) | |
| Race, (n) | |||
| White, (164) | 164 (100) | 121 (74) | |
| Black or African American, (12) | 12 (100) | 11 (92) | |
| Asian,(1) | 1 (100) | 1 (100) | |
| Native Hawaiian or Other Pacific Islander,(1) | 1 (100) | 1 (100) | |
| Other/Not provided/Unknown, (36) | 36 (100) | 31 (86) | |
TEAE-treatment-emergent adverse event; SEA=serious adverse event
Adapted from Clinical trial report
WHO WAS IN THE CLINICAL TRIALS?
Who participated in the clinical trials?
The FDA approved IDHIFA based on evidence from one clinical trial (NCT01915498) of 214 patients with AML whose disease has come back or has not improved after previous treatment(s).
The selected patients had a certain type of mutation (IDH2-mutation) which was confirmed using an FDA-approved test.
The trial was conducted in United States and France.
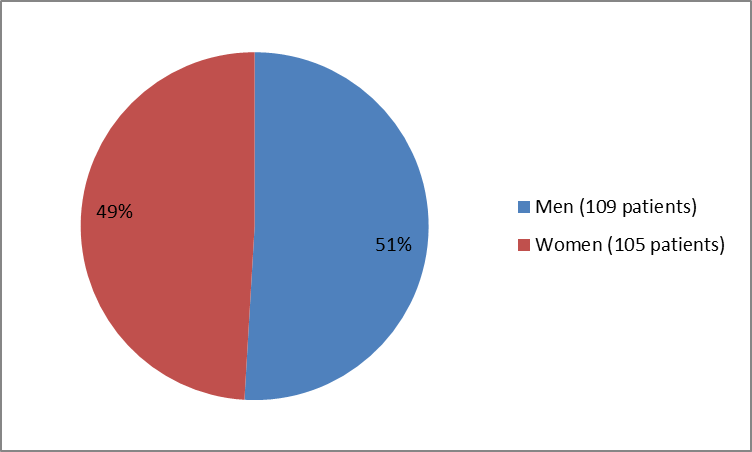
Figure 1 summarizes how many men and women were in the clinical trial.
Figure 1. Baseline Demographics by Sex
FDA review
Figure 2 and Table 1 below summarize the percentage of patients by race in the clinical trial.
Figure 2. Baseline Demographics by Race
FDA review
Table 1. Baseline Demographics by Race
| Race | Number of Patients | Percentage |
|---|---|---|
| White | 164 | 77 |
| Black or African American | 12 | 6 |
| Asian | 1 | less than 1 |
| Native Hawaiian or Other Pacific Islander | 1 | less than 1 |
| Not reported or Unknown* | 35 | 16 |
| Other | 1 | less than 1 |
* collection of data not allowed by French authority
FDA review
Figure 3 summarizes how many patients of certain age were enrolled in the clinical trial.
Figure 3. Baseline Demographics by Age
FDA review
Who participated in the trials?
The table below summarizes demographics of all patients enrolled in the clinical trial who received IDIFA at recommended dose (safety population).
Table 7. Baseline Demographics of Patients Enrolled in the Clinical Trial (Safety population)
| IDHIFA (N=214) | |
|---|---|
| Sex, n (%) | |
| Men | 109 (51) |
| Women | 105 (49) |
| Race n (%) | |
| White | 164 (77) |
| Black or African American | 12 (6) |
| Asian | 1 (<> |
| Native Hawaiian or Other Pacific Islander | 1 (<> |
| Other | 1 (<> |
| Not provided or Unknown* | 35 (16) |
| Ethnicity, n (%) | |
| Hispanic or Latino | 20 (9) |
| Not Hispanic or Latino | 136 (64) |
| Not provided* | 58 (27) |
| Age Categories, n(%) | |
| Age (years) Median (Min, Max) | 68 (19, 100) |
| ≤ 65 years | 85 (40) |
| >65 years | 129 (60) |
| ≥75 years | 51 (24) |
| Geographic Region n (%) | |
| US | 178 (83) |
| France | 36 (17) |
* collection of data not allowed by local authority
FDA Review
How were the trials designed?
There was one trial that evaluated the benefit and side effects of IDHIFA in patients with AML whose disease has come back or has not improved after previous treatment(s). All patients had a certain type of mutation (IDH2-mutation) which was confirmed using an FDA-approved test.
Patients received IDHIFA once a day until disease worsened or unacceptable toxicity.
The benefit of IDHIFA was evaluated by measuring:
- how many patients reached complete remission (no evidence of disease) with full or partial recovery of blood counts after treatment,
- how long those patients remained in remission,
- and the percentage of patients who no longer required transfusions after treatment.
How were the trials designed?
The safety and efficacy of IDHIFA were established in one open-label, single-arm, multicenter, two-cohort clinical trial of 214 adult patients with relapsed or refractory AML and an IDH2 mutation.
Patients received IDHIFA orally at dose of 100 mg daily until disease progression or unacceptable toxicity.
The efficacy was established on the basis of the rate of complete response (CR)/complete response with partial hematologic recovery (CRh), the duration of CR/CRh, and the rate of conversion from transfusion dependence to transfusion independence.
GLOSSARY
CLINICAL TRIAL: Voluntary research studies conducted in people and designed to answer specific questions about the safety or effectiveness of drugs, vaccines, other therapies, or new ways of using existing treatments.
COMPARATOR: A previously available treatment or placebo used in clinical trials that is compared to the actual drug being tested.
EFFICACY: How well the drug achieves the desired response when it is taken as described in a controlled clinical setting, such as during a clinical trial.
PLACEBO: An inactive substance or “sugar pill” that looks the same as, and is given the same way as, an active drug or treatment being tested. The effects of the active drug or treatment are compared to the effects of the placebo.
SUBGROUP: A subset of the population studied in a clinical trial. Demographic subsets include sex, race, and age groups.